Diagnosing Wound Infections: Types of Wound Cultures
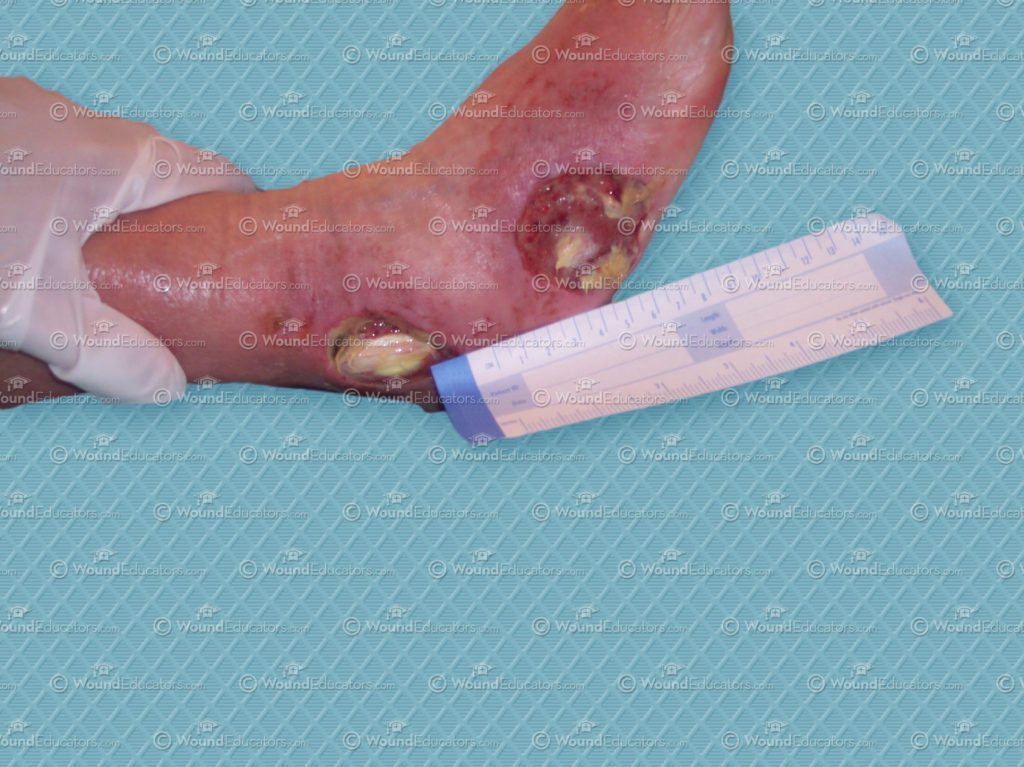
Your patient arrives a day early for a scheduled dressing change. As you prepare to remove and change the bandage, the patient tells you that he has had increased pain in the days since the last dressing change, and also an increased amount of drainage which you can see for yourself. You take the dressing off and note that the wound has an increased amount of thick greenish-colored exudate with a mildly foul odor. You also note that the periwound area is reddened with increased edema since last visit. You suspect that the wound has become infected.
Although you would probably be correct in suspecting that the wound has become infected, suspicion alone is not sufficient to diagnose infection. Wound cultures are needed to identify the presence (or absence) of infection.
Types of Wound Cultures
A wound culture is the process of placing a microorganism in an environment conducive to cell growth, such as a broth or an agar plate. There are several different types of wound cultures:
Tissue biopsy involves removal of a small sample of tissue from a wound for examination. It is usually performed by a physician but may also be performed by other trained professionals.
Bone biopsy is a type of tissue biopsy; a bone biopsy is the most accurate way to diagnose infection in the bone (osteomyelitis). Bone biopsies are always performed by physicians.
An advantage of tissue biopsy is that it is a very reliable method of wound culture, especially compared to swab cultures. However, there are disadvantages, including risk of bleeding and introduction of infection due to the fact that it is an invasive procedure.
Swab cultures sample the wound surface, along with small amounts of wound fluid expressed from the wound or obtained from areas of tunneling or undermining, in order to quantify the amount/number and type of bacteria present on a wound (the wound needs to be cleansed before swabbing takes place). Swab cultures can be performed by nurses and other health professionals without a physician’s order when infection is suspected.
Swab cultures are the most commonly used method to culture wounds due to the fact that they are easy to perform, do not cause trauma to the wound bed and avoid a surgical procedure that can result in complications. A disadvantage of swab cultures is that they only sample the surface of wounds, therefore results may reflect only surface contamination or colonization.
Fluid aspiration utilizes a small needle to withdraw fluid within the wound for laboratory analysis. This procedure is usually reserved for physicians.
The advantage of fluid aspiration is that samples bacteria present in the wound tissue, rather than assessing bacteria on the wound surface. They are most useful for diagnosing wound infections in abscesses. A disadvantage is that there must be sufficient fluid present in order to perform fluid aspiration. There are also certain risks involved, such as introducing infection along the needle tract, formation of a fistula, and damage to underlying structures from introduction of the needle.
Diagnosing wound infection is an important part of wound care, as infection can cause a wound to stall in the healing process, or even enlarge. Remember the signs of infection (redness, swelling, increased drainage, increased pain) and be proactive in assessing and diagnosing infection.
If you enjoy learning about wound care, consider becoming certified in wound management. Wound Educators is the foremost online wound education forum, offering wound certification courses for healthcare professionals.
Sources:
Meyers, B (2008). Wound Management: Principles and Practice. 2nd edition. Pearson Prentice Hall. Upper Saddle River, New Jersey. pg. 100-102.