Anatomy of the Skin – Overview
Anatomy of the Skin
A good understanding of skin anatomy is necessary to be able to evaluate wound depth and the extent of damage to the tissues, as well as in the assessment of wound healing. How much do you remember (or how much have you forgotten!) about the anatomy of the skin?
The skin varies in thickness from .05 mm to 6 mm, with the thinnest layer located on the eyelids and the thickest on the palms and soles of the feet. Your skin weighs approximately one-sixth of your total body weight, making it the largest organ in (or, more accurately on) your body. It receives one-third of your cardiac output when you are at rest.
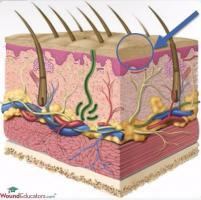
The skin is composed of two layers, the epidermis, and the dermis. Under the dermis is subcutaneous tissue. Deeper structures located under the subcutaneous tissues include muscle, bone and other important structures that you must be able to recognize.
The Epidermis
The epidermis is the outermost layer of your skin. It is the layer that is visible to the world and thus is important to your sense of self. The skin is constantly growing. The epidermis is comprised of five layers. New cells (keratinocytes, which produce keratin) are formed in the bottom layer and make their way up to the top layer, where they are shed. This process takes two to three weeks in total. The layers of the skin, from bottom to top, include:
- stratum basale– a single row of newly formed keratinocytes
- stratum spinosum– so named because of the spiny appearance of keratin filaments under the microscope, this layer is composed of several rows of maturing keratinocytes
- stratum granulosum– this layer consists of three to five rows of keratinocytes with increasingly higher concentrations of keratin
- stratum lucidum– consists of a few layers of dead cells which are clear when viewed under the microscope (hence the name)
- stratum corneum– this is the outermost “horny” layer of the epidermis, consisting entirely of dead cells waiting to be shed; this layer can be up to 30 cells thick, making it the thickest layer of the epidermis by far
Several cells within the epidermis perform specialized functions. Merkel cells provide information to your brain regarding light touch. Melanocytes are responsible for the color, or pigment, of your skin and protect your skin from radiation effects. Langerhans’ cells help to fight infection and dwell in the deeper layers of the epidermis. In addition to these specialized cells, several appendages are also present in the epidermis, including hair follicles containing sebaceous glands. Sebaceous glands secrete sebum, which helps to lubricate our skin and hair. Our hair contributes to cosmesis. Sudoriferous glands are also present in the epidermis and secrete sweat containing metabolic waste products, salt, and water. These waste products make their way to the skin surface via sudoriferous ducts. Nails consisting of hardened keratin are also present in the epidermis and help to protect the ends of our fingers and toes.
The epidermis is not just a pretty face, or the face you present to the world! It performs many vital functions. It provides a barrier to microorganisms and other harmful substances. It plays a role in converting sunlight into vitamin D by converting 7-dehydrocholesterol into cholecalciferol when your skin is exposed to the sun. The skin also helps to regulate fluid, assists us in gathering information that is sent to the brain regarding light touch, helps to regulate our body temperature and assists with excretion of waste products.
Next, we will be looking at the dermis, subcutaneous tissues, and deeper tissues.
Interested in certification? Wound certification can boost your career and, even more importantly, help you to more effectively manage your patients’ wounds. View our wound care certification courses to learn more.
Editors Note: This post was originally published in March 2014 and has been revamped and updated for accuracy and comprehensiveness.

It would be helpful to have video of “live” wounds that highlight the differences between granulation tissue and non-granulating dermal tissue versus superficial dermis vs subutaneous tissue in wound beds.
Great recommendation. I will present this to our team and hopefully have a video like this available to the public in the near future. Our wound care certification courses do have videos like this which are very useful in helping students understand the various tissue types. thanks for posting.
Thanks Laurie,I enjoy relearning the basics that are easily forgotten after that test they were studied for in nursing school.I work with Hospice and that presents special problems with wound care and the focus on comfort instead of healing primarily. Although when I am able to make a difference in a terminal patients life by doing the right thing with the wound it is very rewarding.I love wounds in that they will tell you what you need to do in order to make them well again.As well as show you real quick if you are doing the correct treatment or not.I will look forward to reading more about skin with your next post. Regards David Arnold
Hi David, Your work in hospice is amazing and I am sure you are a very gifted and compassionate nurse. The quality of life for hospice patients can be greatly improved with advanced knowledge in wound care, pain management and wound dressings. Many of our students are hospice nurses who become wound care certified. Have you considered wound care certification?
am an lpn and will like to continue my education on wound care to any lever. can you please tell me the steps from lpn wound care nurse to the highest level.
Hi Regine, I admire your desire to improve your wound care education. Advanced wound care training and wound care certification can provide a tremendous benefit to your patients and your professional career. I recommend that your review our LPN Wound Care Certification Course and contact us with any questions.