Mistaking COVID-19 Symptoms as Pressure Injuries
Patients with COVID-19 may be especially susceptible to unavoidable pressure injuries because of the way the COVID-19 virus interferes with the human body’s normal processes.
Background: What is Considered an Unavoidable Pressure Injury?
The National Pressure Ulcer Advisory Panel (NPUAP) has defined an unavoidable pressure injury as one where the proper evaluation was completed and the interventions were consistent with the patient’s needs, goals, and standards of practice, yet a pressure injury developed despite reasonable care. [1]
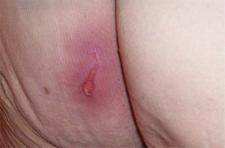
Why Pressure Injuries May be Unavoidable for Some COVID-19 Patients
COVID-19 causes coagulopathy, a condition in which the blood’s ability to coagulate (form clots) is impaired. While the coagulopathy reported is not completely understood, it does involve the body’s largest organ – the skin. In the worst cases, patients with COVID-19 experience microvascular thrombosis, causing unavoidable (and rapidly deteriorating) pressure injuries despite proper support systems and precautions taken.
While it should not be interpreted that COVID-19 automatically causes pressure injuries, it is something that needs to be monitored, especially in patients with underlying health conditions.
The landscape for what is considered an unavoidable pressure injury is also subjectively changing during COVID-19; the current preventative medical supply shortage, limited hospital space, and overburdened medical staff can exacerbate the prevalence of pressure injuries. Healthcare providers may be forced to take greater risks they would not normally take due to lack of readily available equipment.
Mistaking COVID-19 Symptoms As Pressure Injuries
Conversely, clinics across the world are also reporting a new phenomenon- purple skin, hands, and purple toe lesions. These manifestations are NOT pressure injuries, as the skin was not exposed to pressure. Some clinicians are calling this condition “COVID toes”.
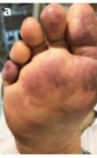
The reported changes “included rashes, acral areas of erythema with vesicles or pustules (pseudo-chilblain), other vesicular eruptions, urticarial lesions, maculopapular eruptions, and livedo or necrosis. The purpuric skin lesions showed a pauciinflammatory thrombogenic vasculopathy, with deposition of Complement 5b-9 and Complement 4d in both grossly involved and normally appearing skin.” [2]
Purple skin discoloration not exposed to pressure needs to be monitored and more accurately characterized as COVID-19 skin manifestations.
The full extent of COVID-19 symptoms are still being analyzed and understood. Any clinician with additional case reports is being asked to submit to the American Academy of Dermatology COVID-19 Dermatology Registry.
Resources
[1] https://cdn.ymaws.com/npiap.com/resource/resmgr/white_papers/Unavoidable_in_COVID_Pandemi.pdf
[2] https://cdn.ymaws.com/npiap.com/resource/resmgr/white_papers/COVID_Skin_Manifestations_An.pdf
