Types of Pyoderma Gangrenosum
Pyoderma gangrenosum is a rare but serious ulcerating skin disease, which can present in many forms and to a variety of health professionals. This means a diagnosis of the condition is often delayed, lead to serious clinical consequences for the patient. [1]
Pyoderma gangrenosum presents most commonly on the lower legs, particularly in the pretibial area. However, the condition is also sometimes seen on other locations in the body, including the breast, hand, trunk, head and neck, and peristomal skin. [2]
Four Types of Pyoderma Gangrenosum
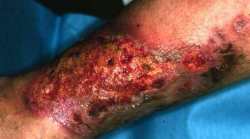
- Ulcerative Pyoderma Gangrenosum (sometimes also known as ‘classical’ pyoderma gangrenosum) – Ulcerative pyoderma gangrenosum is the most common presentation of the condition, and the initial lesion is often described by patients as an insect bite as it has the appearance of a small, red papule or pustule.3 However, the lesion grows rapidly into a larger ulcer with associated tissue necrosis and enlargement of the area. The surrounding skin becomes erythematous and the ulcer borders are typically undermined and violaceous or blue in color. The ulcers tends to develop a purulent cover, which can rapidly become malodorous due to secondary infection. The patient typically experiences intense pain due to ulcerative pyoderma gangrenosum.1
- Pustular Pyoderma Gangrenosum – Pustular pyoderma is a rare superficial variant of the disease that tends to occur on the trunk and extensor surfaces of the limbs. A pustule or group of pustules tends to coalesce and ulcerate, but not to progress further in the way of ulcerative pyoderma gangrenosum. However, the patient usually suffers a painful pustule that may persist for months.1
- Bullous Pyoderma Gangrenosum – Bullous pyoderma gangrenosum is a superficial variant of the condition which typically presents as concentric bullous areas on the upper limbs and face. Bullous pyoderma is commonly associated with an underlying hematological malignancy.1
- Vegetative Pyoderma Gangrenosum – Another superficial variant is vegetative pyoderma gangrenosum which tends to occur as a single lesion in patients who are otherwise well. This form typically responds to topical treatment.1
- Etiology – The etiology of pyoderma gangrenosum is not well understood, but is thought to involve an inappropriate immune response to a number of unidentified factors.1-3 Since inflammatory bowel disease is the most common underlying disorder, cross-reacting antigens in the bowel and the skin could be responsible for secondary cutaneous manifestation.2 Cellular analysis has shown aberrant neutrophil activity in patients with pyoderma gangrenosum, with tissue necrosis caused by unchallenged neutrophil infiltration.2
Because of the variety of ways in which the types of pyoderma gangrenosum can present, it can be a difficult condition to identify. However, delayed diagnosis has serious consequences in terms of patient morbidity and quality of life. Therefore, pyoderma gangrenosum is an important condition to study. To learn more about this condition, and other rare but potentially serious pathologies, consider becoming certified in wound care.
Learn More With Our Wound Care Education Options
Interested in learning more about the types of pyoderma gangrenosum and other wound care topics? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- Brooklyn T, Dunnill G, Probert C. Diagnosis and treatment of pyoderma gangrenosum. BMJ. 2006;333:181-4.
- Wollina U. Pyoderma gangrenosum–a review. Orphanet J Rare Dis. 200715;2:19.
- Jackson M, Callen JP. Pyoderma gangrenosum. Medscape March 2010 (available at http://emedicine.medscape.com/article/1123821-overview#a0199).

having an iodne base weekly, how long will that last expering burning and sting along with some nerve pain taking gabapetin 300mg 3 times daily how long before this goes away and how long am i going to be with this? also taking dapsone daily
As you probably know by now ,stinging from iodine will last until the wound has scabbed over or new skin has grown over the wound.