Abnormal Wound Healing (Part 2)
In part one of this series, we discussed abnormal wound healing in terms of too much or too little inflammation (absence of inflammation versus chronic inflammation). The inflammatory phase is not the only phase of healing in which healing can be derailed- it can also happen in the proliferative phase, where granulation takes place.
Hypogranulation (nonadvancing wound edge)
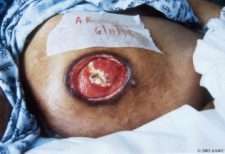
Hypogranular wounds fail to build enough granulation tissue to fill the wound bed. This results in a pothole-type wound. Why does this occur? It happens when there is a lack of support owing to the absence of a granular matrix. Repair is suspended because epithelial cells cannot ‘bridge the gap’ to achieve wound closure. Occasionally, epithelial cells will continue to multiply and will attempt to turn the corner, migrating down the sides of the pothole. When they reach the floor (or each other) they form a lip over the pothole edge, called an epibole. The keratinocytes mistakenly believe that migration has been successful, thus epithelialization comes to a halt. Other causes of hypogranulation may include:
- formation of scar tissue around the perimeter of the wound
- presence of senescent cells (present in chronic wounds)
- wound dehydration
- heavy wound bioburden
- local tissue hypoxia
- repeated trauma from dressing changes or improper wound dressings
Hypogranulation occurs most frequently in diabetics and individuals who are poorly nourished. How are these wounds addressed? In these wounds, the goal is to protect and enhance granulation. This can be achieved by one or more of the following measures:
- wiping the wound edges gently with gauze during each dressing change- this prevents epithelial cells from migrating inappropriately down the sides of the wound, allowing granulation tissue to form unimpeded
- packing the wound- filling a pothole-type wound lightly is thought to decrease the risk of premature epithelialization
- serial debridement- debridement decreases wound bioburden; it is also thought to facilitate healing by restarting the inflammatory process in senescent cells that lay within the wound bed
Hypergranulation
As opposed to hypogranulation, which results in a pothole-like wound, hypergranulation results in a mound of granulation tissue that extends above the skin surface. In hypergranulation, the formation of granulation tissue continues after the wound defect has been filled. Too much granulation tissue actually deters epithelialization because the epithelial cells have difficulty climbing up the mountain of granular tissue. This results in a rolled wound edge which is quite easily identified.
The approach to hypergranulation is two-pronged: prevention and resolution.
- prevention- to prevent hypergranulation from occurring, it is important to protect the fragile epithelial cells from any form of trauma, as may occur when dressings are changed too often, the wound is allowed to become macerated, adhesives are used or whirlpool baths are used inappropriately. Hydrocolloids have been linked to hypergranulation and should be discontinued at the first sign.
- resolution- once present, hypergranulation tissue may be resolved in one of three ways: application of pressure over the abnormal tissue (which results in ischemia of the abnormal granulation tissue), use of a silver nitrate stick on the hypergranular tissue or surgical excision of the hypergranular tissue.
Understanding what can go wrong during wound healing can help the astute clinician in preventing these complications, or at least identification of the problem early on. If you are interested in learning more about wound care and wound care management, Wound Educators offers online training to prepare you to become a certified wound care specialist. Visit www.woundeducators.com to learn more.
Sources
Myers, B. (2008). Wound Management Principles and Practice. 2nd Edition. Pearson Prentice Hall, Upper Saddle River, New Jersey. pg. 19-20.
McGrath, A. (2011). Overcoming the challenge of overgranulation. Wounds UK, 7 (1); pg. 42-49. http://www.wounds-uk.com/pdf/content_9839.pdf

please i want to know all the types of abnormal wound healing
Hi Dorcas, You can view additional posts about abnormal wound healing here: https://woundeducators.com/?s=ABNORMAL+WOUND+HEALING+
I am worried that my open wound is hypergranulating. It is raising above the surface of my skin and bleeding a little. My doctor can’t see me for 2 days. Wondering if I should go to ER. I am 18 weeks pregnant and got the wound from hormone injection in my hip that had to be cut open and debrided for several weeks. It is taking forever to heal.
Jeanine,
I would use your intuition and do what’s best you and your baby. Better to be safe than sorry! You can search for certified wound specialists in your area here: https://portal.abwmcertified.org/ABWMweb/Directory/ABWMcontent/Directory.aspx
Best of luck!
I had open heart surgery 18 months ago. I have a wound between my breast that will not heal.. it’s very painful. I had wires removed . I had wound cut out and vacuum treatment. Followed by debridement and silver nitrate treatment. Nothing helps. Oozes green gray pus constantly. They are planning a flap procedure. YOUR THOUGHTS?????