Abnormal Wound Healing (Part 3)
We’ve already discussed problems with wound healing that occur during the inflammatory and proliferative phases of wound healing. Next we’ll take a look at what can go wrong during the maturation and remodeling stage of wound healing.
Hypertrophic Scarring
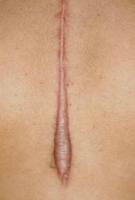
Hypertrophic scarring occurs when there is an overproduction of immature collagen during the maturation phase of wound healing. When this occurs, you will see raised, red fibrous lesions that do not extend beyond the confines of the original wound. This type of abnormal scarring is most likely to occur in chronic wounds that are large and/or infected, or in wounds that cross a line of tension in the skin. Hypertrophic scarring is common in burn injuries due to the prolonged proliferative phase associated with burns. Individuals with darker skin are more likely to develop hypertrophic scarring than individuals with lighter skin.
Managing hypertrophic scarring may include one of the following:
- Compression garments- garments worn for 23 hours a day cause local ischemia, which can help to modify the scar
- Silicone gel sheets/pads- these are thought to increase temperature under the sheets or pads, which in turn increases the rate of collagen lysis
- Scar mobilization- this is performed by physiotherapists and may or may not include ultrasound
- Steroid injections- performed by physicians, repeated steroid injections can help to modify scar tissue
- Topical agents- topical agents may be used to assist with collagen reorganization (i.e. allium cepa or Mederma)
- Surgery- surgery is performed to decrease tissue tension, which can decrease the rate of collagen synthesis
Keloids
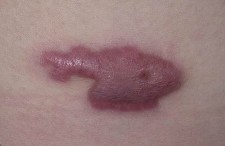
Keloids are similar to hypertrophic scars, except that they extend beyond the edges of the original wound. Like hypertrophic scars, they are caused by an excess of collagen synthesis. Keloids are far more common in individuals with dark pigmentation. Keloids are unlikely to regress without treatment. Keloids often undergo a period of growth followed by a period of stabilization, after which they may grow intermittently. Tissue trauma is often the trigger for keloid formation (i.e. surgery, burns, ear piercing or tattoos). There is a tendency for keloid formation to run in families. Keloids appear as nodular masses arranged in clusters or swirls of collagen fibers.
Treatment for keloids includes:
- Steroid injections
- Surgical excision
- Radiation
- Compression garments
- Z-shaped incisions (also called Z-plasties) which are used to decrease tissue tension in the affected areas
Contractures
A contracture is caused by shortening of scar tissue, which results in deformity. They occur most often in patients who have wounds that cross a joint, such as burns. Patients will often position the wounded extremity in a position of comfort to decrease pain and tension on the healing area and the surrounding soft tissues. Unfortunately, this leads to adhesions and shortening of muscles, joint capsules and tendons, which eventually inhibits the patient’s ability to move the affected area effectively.
Prevention is the key to avoiding contractures. Clinicians should identify clients at risk, such as burn patients and patients with wounds crossing one or more joints. Range of motion exercises can be taught to patients to decrease the risk of developing contractures. Patients should be advised to avoid adopting a position of comfort. Splints may be necessary for ideal positioning.
Wound Dehiscence
Wound dehiscence occurs when there is insufficient scar tissue formation. Wound margins separate due to decreased tensile strength and inadequate collagen formation. Diabetic patients, steroid users and patients who have poor nutritional status are at higher risk of wound dehiscence. Abdominal wounds are particularly prone to dehiscence because the abdomen is a high tension area.
As we have learned in the last three articles, abnormal wound healing can occur due to problems in the inflammatory phase, the proliferative phase or the maturation/remodeling phase. Clinicians must be cognizant of the issues that can arise during healing and understand the risk factors that may put their clients at higher risk for developing these issues.
View Related Articles
Abnormal Wound Healing (Part 1)
Abnormal Wound Healing (Part 2)
If you are interested in learning more about wound healing and wound management, Wound Educators has a wealth of resources available. Interested in becoming a certified wound care specialist? Visit woundeducators.com to learn more.
Meyers, B. (2008). Wound Management Principles and Practice. 2nd edition. Pearson Prentice Hall. Upper Saddle River, New Jersey.
Abnormal wound healing. DermNet NZ. Updated December 2013. http://www.dermnetnz.org/doctors/wound-healing/abnormal-healing.html

I missed my WCC test by 2 the first time and 4 the second time do u have any suggestions how to study this to pass
Hi Barbara, I recommend that you take the wound care certification course offered by woundeducators.com. Our courses are 50-60 hours and allow for 6 months access. Wound care is a very complex topic and a 4 day seminar course does not provide enough time to adequately prepare for the certification exam.