Local Factors Affecting Wound Healing
There are several local factors that can affect wound healing. Circulation, sensation and mechanical stress are among the most common local factors that have a bearing on healing.
Circulation
Palpable pulses do not always indicate sufficient circulation. They indicate that the major vessels have good flow, but they do not indicate that the microcirculation is adequate, which may mean that blood flow to the area of injury is insufficient. Conditions such as diabetes and PVD (peripheral vascular disease) that affect microcirculation can slow or impair wound healing.
Circulation can also be affected by the autonomic nervous system. Conditions that result in vasoconstriction of peripheral blood vessels, such as cold, pain and fear, can impair wound healing. For this reason, it is important to be alert and monitor for signs and symptoms of these three conditions in patients with wounds. Pain is common in individuals with wounds and should be treated aggressively when present. Should non-pharmacological, topical and/or over-the-counter pain remedies fail to relieve a patient’s pain, the patient’s physician should be notified. Fear can be alleviated by explaining all treatments before they are performed and answering the patient’s questions beforehand. Clinicians should endeavour to ensure that the wound (and the patient) remain at a stable or constant temperature. This can be achieved by utilizing blankets and heat lamps when the patient (or the wound) is exposed to cool temperatures. Dressings that can remain in place for several days, rather than being changed daily, can help to maintain the wound bed at a constant temperature to promote healing.
Sensation
The inability to sense pain and/or pressure can also impede wound healing. When an individual cannot feel or sense pressure or pain, they are not capable of discerning when tissue damage is occurring. This may lead to underestimation of the extent of tissue damage and/or a delay in seeking medical treatment. This happens often in patients with diabetes who develop blisters or areas of pressure on their feet due to ill-fitting shoes. A small blister can morph into a large open area quickly without the patient being any the wiser because they have poor sensation in their feet. This is one reason why diabetics should be taught to examine their feet routinely and visit their podiatrist regularly.
Another issue caused by decreased sensation is that individuals with the inability (or poor ability) to sense pain and pressure may continually traumatize a wounded area unknowingly or inadvertently. For example, the diabetic patient in the example above may continue to wear tight-fitting shoes even after developing a blister because they do not feel the pain that individuals with intact sensation would feel in the same situation. Thus, they continually traumatize the injured area.
Mechanical Stress
Any form of mechanical stress on a wound will delay healing, so minimizing mechanical stress will improve or enhance healing. Mechanical stress is any stress that produces shear, pressure, or friction. For example, a patient who is confined to a wheelchair will experience pressure on his coccyx. If the patient develops a pressure ulcer to the coccyx, continuing to sit in the wheelchair will impair wound healing. Offloading (relieving mechanical pressure) will enhance healing. In this case, the patient may be required to lay in bed on his side for a time to allow the coccyx wound to heal. The patient may also require a different wheelchair cushion that relieves pressure on the coccyx area.
As can be seen, local factors such as circulation, sensation and mechanical stress can influence both the development and the rate of healing of wounds. If you are interested in learning more about factors that influence wound healing, visit Wound Educators, where you can find all the information you need on wound education and wound care certification.
Sources:
Meyers, B. (2008). Wound Management: Principles and Practice. 2nd edition. Pearson Prentice Hall, Upper Saddle River, New Jersey. pg. 29-30.
Hess, T. (2011). Checklist for factors affecting wound healing. Advances in Skin & Wound Care; 24(4): p 192

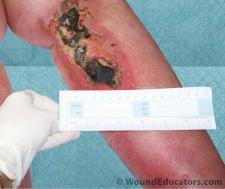
I have two wounds on my right foot and they are healing process is slow. I am in Broward House, which is a wound care facility. I just seen.orthopedic specialist for right knee replacement but doctors will not do surgery until my right foot staff infection is completely healed. My case manager at Broward House told me that I would be discharged before I am completely healed. Do you any advice for me
Respectfully submitted
Richard Martin
954-263-9358
Hi Richard,
I recommend that you contact a certified wound care specialist in your area and request a consult. You can find local certified wound care specialists here. Good luck!
hello
Thanks for your information.I am a nurse from Iran and i work in wound care and management but my knowledge is not academic and ilearned by myself.would you please sent any article that can help me in this fild.
thanks
Hi Abdoreza,
I recommend that you read our blog articles and visit our resource area for free information pertaining to wound care management. Form a more in-depth education I highly recommend our RN wound care certification course.
Best Regards,
Laurie
Hi,is Margarita Gonzalez from Puerto Rico:
Right now I’m working in a Trauma Center.Just want to know the classification of a second degree burn when the skin haven’t been debrided and has a hard crust. The color is like slough. Can be classified like slough tissue in a burn person?
Hi Margarita, “second degree” is the classification for the burn and “slough” describes the tissue. Here is a good reference that describes burn classification and tissue types.