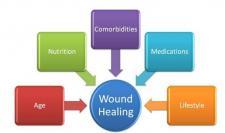
Systemic Factors Affecting Wound Healing
In addition to local factors that can influence wound healing, such as circulation, sensation and mechanical stress, there are a number of systemic factors that can also play a role.
Aging– aging causes many changes that adversely affect the skin and its ability to heal and regenerate itself. In terms of ability to heal, as we age our immune function deteriorates, as evidenced by fibroblast and macrophage impairment. Our ability to produce collagen is decreased, and our collagen also becomes weaker. The skin is thinner, leading to an increased risk of tearing and blistering. The skin is also drier, thanks to a decrease in the number of sweat and oil glands. When a wound to the skin occurs, healing is impaired by a decrease in the body’s inflammatory response. The ability to feel and respond to pain is often muted in older individuals, which means that minor trauma to the skin may occur and go unrecognized due to the individual’s lack of sensation. Older patients are more susceptible to infection, and signs and symptoms of infection may be less noticeable. Lastly, older patients often have comorbidities which can further impair wound healing.
Inadequate Nutrition– patients who eat an inadequate diet are at higher risk of infection and delayed wound healing. Carbohydrates, in particular, are the preferred source of energy; if carbohydrates are not available in high enough quantities, the body will burn amino acids from protein for energy. Protein is required for repair and regeneration at the cellular level, therefore protein depletion will result in a whole host of undesirable effects, such as impaired inflammation, poor immune response and altered proliferation, maturation and remodeling responses.
Comorbidities– Tissues require oxygen to survive. Any disease process that interferes with the body’s ability to provide oxygen to the tissues will result in poor wound healing. These conditions might include peripheral vascular disease, anemia and chronic obstructive pulmonary disease. The presence of oxygen is important in all phases of wound healing.
An intact immune system is also necessary for wound healing. Individuals who have altered immunity due to disease will have increased risk of infection and poor wound healing. Immune compromise may be due to conditions such as diabetes or HIV/AIDS, or may be part of the normal process of aging. Chemotherapy and radiation can alter immune function, as can steroid use and poor nutrition.
Any condition that decrease’s an individual’s ability to move can also hinder repair and may lead to skin breakdown. For example, a patient who is unable to roll over in bed may develop pressure ulcers. Movement may be limited by a physical condition, such as stroke or arthritis, or may be restricted due to a medical treatment or device, such as a cast or a restraining device. Patient who are unwilling to move (i.e. in severe pain or suffering from depression) are also at higher risk of developing skin breakdown which may be slow to heal.
Medications– Some medications can affect wound healing. Steroids are one example. High doses of steroids can suppress both the immune system and inflammation (remember, not all inflammation is bad!). Steroids can decrease the synthesis of collagen and impact its strength. Chemotherapy is designed to destroy cells and is always damaging to healing. NSAIDS have also been implicated in a delay in wound healing. It is thought that because NSAIDS decrease inflammation, they can impair wound healing by suppressing the inflammatory phase of healing; however, research has not really borne out this school of thought at least thus far. What is known is that NSAIDS are associated with a decrease in the tensile strength of wounds.
Personal Behavior- patients must sometimes share some of the responsibility when wounds fail to heal or heal slowly. This is due to personal choices that adversely affect wound healing. Abuse of alcohol often leads to malnutrition, which can impede wound healing. In addition, excessive use of alcohol can lead to injury that might go unrecognized.
Smoking restricts blood vessels, causes platelets to stick together (aggregate) and leads to clot formation and strength. In addition, the carbon monoxide inhaled while smoking binds to hemoglobin, which reduces the amount of oxygen available to the tissues that desperately need oxygen to heal.
In order to help patients to heal their wounds, clinicians must ask questions regarding nutrition, medication and lifestyle factors that might adversely affect healing. Age cannot be modified, but should be kept in mind when designed a wound management plan.
Want to learn more about wound healing and wound management? Visit Wound Educators to learn how you can obtain your wound care certification, a career move which can boost your standing among your colleagues, not to mention your salary.
Sources
Myers, B. (2008). Wound Management: Principles and Practice. 2nd edition. Pearson Prentice Hall. Upper Saddle River, New Jersey.
Thomas Hess, C. Checklist for factors affecting wound healing. Advances in Skin and Wound Care, 24(4): pg. 192.

The topic of wound healing interest me so much. I would like to have knowledge and skill for this, something like I have to do in the future. Can you help me attain this education? Where do I have to go to get this?
Visit our wound care certification courses page for course information or contact us directly.
I like this blog very much so much superb info.
What’s up to all, the contents present at this web site are in fact amazing
for people knowledge, well, keep up the good work fellows.
A gazillion thanks for some great background info! Think my product would make a huge positive impact for people. Although I am not approved by the FDA,too $$$$, I had my product tested at an FDA approved lab! Did this for “surface ostrich wounds,rashes etc. not internal problems. The results were mind-boggling! As far as humans ingesting my product this is the thing that needs the FDA. Hope to hear from somebody with an idea. Many thanks ,Sincerely, Cynthia Lyman
citation?
Our wound care certification courses and
Myers, B. (2008). Wound Management: Principles and Practice. 2nd edition. Pearson Prentice Hall. Upper Saddle River, New Jersey.
Thomas Hess, C. Checklist for factors affecting wound healing. Advances in Skin and Wound Care, 24(4): pg. 192.