Lymphedema Classification and Characteristics
The term lymphedema describes a condition in which lymphatic fluid accumulates in the interstitium causing swelling and a feeling of heaviness or weakness in the affected area, usually the arms and legs.1
Lymphedema Classification
Lymphedema may be classified either as primary or secondary. Primary lymphedema develops as a consequence of a pathologic congenital and/or hereditary etiology, and occurs relatively rarely.2,3 The much more common classification is secondary lymphedema which tends to due to a mechanical injury caused by surgery, radiation, trauma, infection, tumoral blockage, chronic venous insufficiency, immobility, or tourniquet effects, for example.2,3 Once damage has occurred to the lymphatic system, the transport capacity in the affected region is permanently compromised, creating a lifelong risk of lymphedema. Lymphedema has even been known to develop several decades after the initial trauma.4 In the US, the most common cause of secondary lymphedema is previous breast cancer treatment, particularly a combination of axillary surgery and radiation.3
Lymphedema Characteristics
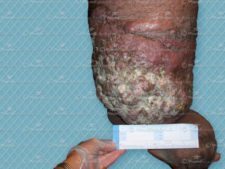
The principal characteristics of lymphedema include a feeling of heaviness or tightness in the limb, which is often accompanied by aching or discomfort, restricted motion, and swelling in part of or the whole of the limb.2 In some cases, swelling may also be observed on the trunk, particularly in the adjacent upper quadrant. Although patients tend to complain of discomfort, severe or prolonged pain is rare. Unlike other inflammatory responses, areas of lymphedema also tend to exhibit a normal skin color and a normal temperature. The swelling involved is usually unilateral, and sometimes includes the dorsum of the hand or foot. The patient may also present with a Stemmer sign, a diagnostic test in which a skin fold cannot successfully be raised.4,5
The characteristics of lymphedema are quite distinct and can usually be observed and noted readily. However, it is important to recognize the signs lymphedema promptly to prevent unnecessary patient discomfort and potentially greater sequelae. Enhanced knowledge and understanding of the characteristics and features of lymphedema can be achieved by pursuing additional professional training, including studying for a certification in wound management.
Learn More With Our Wound Care Education Options
Interested in learning more about wound care certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- Myers BA. Wound management principles and practice. 2nd ed. Upper Saddle River, NJ: Pearson; 2008.
- Lawenda BD, Mondry TE, Johnstone PA. Lymphedema: a primer on the identification and management of a chronic condition in oncologic treatment. CA Cancer J Clin. 2009;59(1):8-24.
- Zuther E. Pathology. In: Von Rohr M, ed. Lymphedema Management: The Comprehensive Guide for Practitioners. New York: Thieme Medical Publishers, Inc; 2005:45-99.
- Brennan MJ, Weitz J. Lymphedema 30 years after radical mastectomy. Am J Phys Med Rehabil. 1992; 71: 12–14.
- Weissleder H, Schuchhardt C. Lymphedema Diagnosis and Therapy. 2nd ed. Bonn, Germany: Kagerer Kommunikation; 1997.

You are most certainly correct that nurses need to be stronger advocates for relief of pain and prevention of pain. My question is what can we do when the physician has no sympathy and refuses to consider either the nurse or the patient in relation to pain? In the meantime the dressing needs to be changed or the wound could get worse.