Lymphedema – Summary
Lymphedema is a notoriously debilitating progressive condition with no known cure. The condition is cause by a defect in the lymphatic system, resulting in an abnormal collection of excess tissue proteins, edema, chronic inflammation and fibrosis. It is estimated that between 3 and 5 million patients in the United States suffer from lymphedema,1 and many report significant pain and a serious impact on quality of life.2
Lymphedema Predisposition
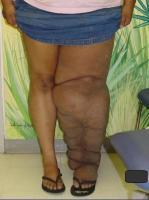
Lymphedema is usually the result of a trauma in the patient’s history, with previous cancer treatment being a major risk factor. Other major types of trauma, burns, a family history of lymphedema, and high body mass index may also predispose to the development of lymphedema.3 As the risk for lymphedema is lifelong, the onset may occur at the time of the initiation of treatment or be delayed, even for several decades.4 Primary lymphedema, which develops as a consequence of a pathologic congenital and/or hereditary etiology and not due to an initial trauma, is also known but is relatively rare.5
Irreversible Tissue Damage
Because no curative treatments exist for lymphedema, and because the condition causes irreversible tissue damage, it is ideally managed by prevention through monitoring of limb girth and volume and patient education.5,6
Lymphedema Treatment Goals
When lymphedema is diagnosed, the goal of treatment is to decrease the excess volume as much as possible and maintain the limb at its smallest size.5,6 The gold standard treatment for lymphedema is complete decongestive therapy (CDT)7 which involves four treatment components: skin and nail care, manual lymph drainage (MLD), compression bandaging, and therapeutic exercise. A major component of CDT is the maintenance phase which consists of life-long self-care to maintain the size of the limb.
Lymphedema represents a major problem for a significant minority of the US population. Its treatment is currently not adequate and its progression is poorly understood. Further information about this difficult-to-manage condition can be gained through the pursuit of additional professional training, including studying for a certification in wound management.
Learn More With Our Wound Care Education Options
Interested in learning more about wound care and certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- Zuther E. Pathology. In: Von Rohr M, ed. Lymphedema Management: The Comprehensive Guide for Practitioners. New York: Thieme Medical Publishers, Inc; 2005:45-99.
- Moffat C, Franks P, Doherty D, et al. Lymphoedema: An Underestimated Health Problem. Q J Med 2003;96:731-738.
- Ridner SH, Dietrich MS, Stewart BR. Body mass index and breast cancer treatment-related lymphedema. Support Care Cancer. 2011 Jun;19(6):853-7.
- Brennan MJ, Weitz J. Lymphedema 30 years after radical mastectomy. Am J Phys Med Rehabil. 1992; 71: 12–14.
- Lawenda BD, Mondry TE, Johnstone PA. Lymphedema: a primer on the identification and management of a chronic condition in oncologic treatment. CA Cancer J Clin. 2009;59(1):8-24.
- Holcomb SS. Identification and Treatment of Different Types of Lymphedema Adv Skin Wound Care 2006;19:103-8.
- International Society of Lymphology. The diagnosis and treatment of peripheral lymphedema. Consensus document of the International Society of Lymphology. Lymphology 2003 Jun;36(2):84-91.

In my experience, physicians are very responsive when presented with solutions and factual information showing “best practices” (i.e. articles, websites, etc.) As nurses we need to be part of the solution and act as a resource for physicians when dealing with than many facets related to wound care, including wound pain.
The less pain academy sponsored by Molnlycke Health Care raises the awareness of dressing related pain and stress by providing latest research, therapies, protocols and best practice in wound care management, dressings, learning, healing: http://www.molnlycke.com:19000/en/Home/