Phases of Wound Healing- Part 2
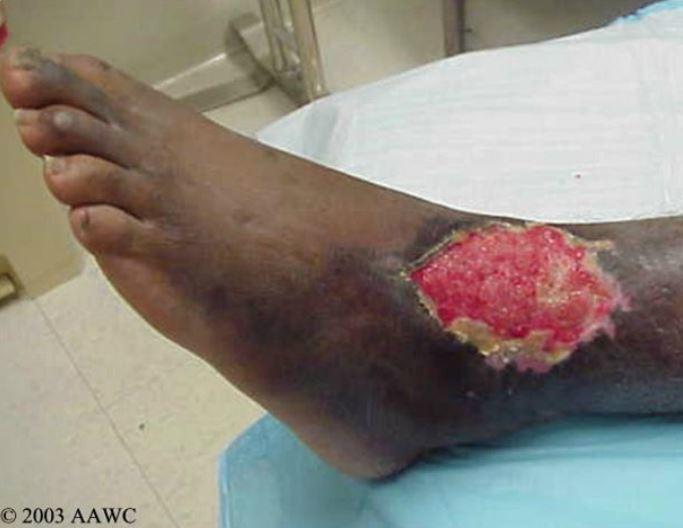
As you might remember from part 1 of this series, there are three phases of wound healing. Last week we discussed the inflammatory phase, which lasts for a few days following injury. Now let’s look at the next two phases: the proliferative and maturation/remodeling phases.
Proliferative Phase
The proliferation phase generally starts within 48 hours of injury (in healthy individuals). It may overlap the inflammatory phase and consists of a series of four events:
- angiogenesis– this is the formation of new blood vessels. Angioblasts, which make up the epithelium of blood vessel walls, grow outward into the affected area. Eventually, they meet and join with other buds and form new capillary loops, which bring nutrition to the area and remove waste products. These buds look like tiny red dots in the wound bed. As they grow and increase in number, they give the healthy wound bed its pink to rosy red appearance
- formation of granulation tissue– MMPs (matrix metalloproteases) are proteases which are formed during the healing process. Their job is to break down debris collected during the inflammatory phase. Granulation tissue is a temporary latticework of connective tissue that fills the void left after the MMPs have degraded the leftover debris.
- wound contraction– fibroblasts within the wound bed transform into myofibroblasts, which pull the wound margins together and decrease the size of the defect; wound contraction is affected by the wound size, shape and depth
- epithelialization– as the wound defect fills with granulation tissue, keratinocytes at the margins of the wounds and epidermal appendages multiply and migrate across the wound bed; keratinocytes elongate, extend pseudopods across the extracellular matrix and pull the parent cells with them as they advance. Chemotactic agents guide keratinocytes toward the wound center. Epithelialization is slowed when there is a lot of cellular debris and when there is poor oxygenation; a clean and moist wound bed facilitates epithelialization
Maturation/Remodeling Phase
Once the wound bed has been resurfaced (epithelialized), the granulation tissue must be strengthened and reorganized to fit the surrounding tissue. Collagen synthesis continues after wound closure- as new collagen is formed, old collagen is broken down by collagenases, which are produced endogenously. Remodeling continues for up to two years following wound closure. The scar tissue is only (at most) 80% of the original tissue’s elasticity and strength.
Wound healing proceeds in an orderly fashion, provided the patient is healthy and their immune system is functioning well. For some, wound healing may stall- and that’s where specialized wound care knowledge comes in handy. If you find wound education interesting, perhaps you should consider online wound care education, such as the wound education offered by Wound Educators, which can prepare you for wound care certification. Contact us today!
Myers, B. (2008). Wound management: Principles and practice. Pearson Education Inc., Upper Saddle River, New Jersey pp 12-16.
Mercandetti, M & Cohen, A. Wound healing and repair. Medscape. Updated April 2013. http://emedicine.medscape.com/article/1298129-overview#a1
Armstrong, D & Meyr, A. Wound healing and risk factors for non-healing. Up to Date. Updated November 2012. http://www.uptodate.com/contents/wound-healing-and-risk-factors-for-non-healing

This is a great article on wound healing. Thanks!
Mindy Ruben
Thanks Mindy, I am happy that you liked it.