Pyoderma Gangrenosum
 Overview of Pyoderma Gangrenosum
Overview of Pyoderma Gangrenosum
Pyoderma is a noninfectious, progressive necrotizing skin condition. The etiology of pyoderma is unclear. Half of patients have a systemic inflammatory condition such as ulcerative colitis, Crohn’s disease, irritable- bowel syndrome, lupus, or rheumatoid arthritis. About a quarter of pyoderma cases begin after some sort of trauma or surgery. But another quarter have an insidious onset. Pyoderma most frequently affects patients who are middle aged. The pathology of pyoderma gangrenosum is poorly understood, but is believed to be due to neutrophil dysfunction.
Presentation
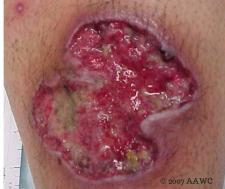
The classic presentation of pyoderma gangrenosum begins as a small, very painful papule, vesicle, or pustule on the lower extremities and/or trunk. While a single lesion is possible, generally there is a cluster of ulcerations that rapidly expands. Pyoderma rapidly progresses to full-thickness ulcerations with irregular, violaceous borders which have purulent and hemorrhagic exudates. Undermining is common. The wound bed is eschar- or slough-covered and the wound edges may be rolled. The periwound is indurated or boggy. The patient may also have fever, malaise, or myalgia. Pyoderma lesions are erythematous due to inflammation, but may also have a blue hue from epidermal necrosis.
Treatment
Immunosuppressive and anti-infective agents are commonly prescribed. Corticosteroids are used to control inflammation. Local wound care includes gentle and limited debridement of slough and necrotic tissue. Extensive sharp or surgical debridement is contraindicated, because it increases the inflammatory response leading to severe exacerbations. Topical antimicrobials are indicated for sensitive bacterial infections. Gauze or moisture-retentive dressings should absorb wound exudate and protect the surrounding tissue. Extremity wounds may benefit from elevation and gradient compression. Negative- pressure therapy and hyperbaric oxygen have been used with some success. Wounds that have stabilized with medication have been treated successfully with skin grafting. Wound healing is extremely slow. Because recurrence is common, physicians generally continue pharmacological management for 6 to 12 months after wound closure.
If you would like to learn more about the etiology and treatment of atypical wounds, consider taking a wound care certification course. Not only will you improve your education and career options, you will also improve the outcomes of your patients.

excellent and want more cme.
If it is truely PG I will do a trial of topical triamcinolone cream if there is vast improvement over a week I will consider injecting kenalog into the boarders of the wound. Hurts but heals in a week or two. I have personally had pretty good luck with this treatment option.