Venous Insufficiency Ulcers – Characteristics
Venous insufficiency leg ulcers are the most common type of leg ulcer, accounting for 70% to 90% of all ulcers. Of the remaining ulcers, an estimated 10% to 15% are due to combined venous and arterial insufficiency. Women are three times more likely than men to have a venous- insufficiency ulcer. The risk of ulceration is 7 and a half times greater in individuals over the age of 65.
Pain
Individuals with venous insufficiency and venous-insufficiency ulcers commonly complain of dull, aching leg pain or “heaviness.” The cause of this pain is venous hypertension and the resulting peripheral edema. The pain is usually increased with dependency, and relieved by elevation or compression. Patients typically report a decrease in pain both at night, due to a decrease in gravity while in bed, and first thing in the morning, due to edema reduction overnight. Many patients report increasing leg heaviness and aching as the day progresses. This results from prolonged dependent positioning, such as sitting or standing. Pain may be severe in the presence of infection or coexisting arterial insufficiency. Patients with diabetic neuropathy are unlikely to complain of pain associated with their wounds because they have decreased sensation
Location
Venous-insufficiency ulcers are usually located on the medial aspect of the lower leg or medial malleolus. It is also common to find venous ulcers in areas exposed to trauma, such as the anterior shin. Venous ulcerations do not occur on the plantar aspect of the foot, and rarely occur above the knee.
Presentation
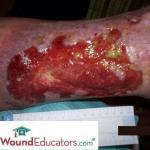
Venous-insufficiency ulcers are generally superficial, irregular in shape, and have moderate- to- high amounts of drainage. If the dressing does not absorb enough wound drainage, the wound edges will be white and fragile due to maceration. The wound bed contains beefy, red granulation tissue but may take on a ruddy appearance. A thin, yellow fibrous coating may cover the wound bed, giving it a glossy look.
Associated Skin Changes
Venous insufficiency is often associated with many skin changes. Cellulitis, Dermatitis and dry, scaling skin” which may cause intense itching are common. Superficial varicosities and evidence of previous ulceration may be present. Lower- extremity edema is usually always present. In cases of long-standing venous insufficiency, the edema may become firm or indurated. Initially, skin changes may include a subtle erythema. With chronic venous insufficiency, the skin becomes stained and more darkly pigmented, due to hemosiderin deposition. Hemosiderin is a by-product of the breakdown of red blood cells, which have been forced into the interstitium by venous hypertension. The term lipodermatosclerosis is used to describe the hyperpigmentation and accompanying erythema, induration, and plaque-like structural changes that occur due to long-standing venous insufficiency. The skin and subcutaneous tissues are more fibrotic and less elastic than healthy tissue.
Pulses
Pedal pulses are generally present and normal in patients with venous ulcers. However, peripheral edema resulting from venous insufficiency may make pedal pulses difficult to palpate. (:) ) In addition, it is not unusual to have coexisting arterial disease, which may decrease pedal pulses. If pulses are not normal, an ABI should be performed to assess for arterial insufficiency.
Temperature
It is not uncommon for cellulitis or edema from venous hypertension to cause a mild increase in the affected extremity’s skin temperature. Local warmth may also be the result of ulcer infection.
Read additional blog posts to learn more about venous insufficiency ulcers.
For more in-depth knowledge about venous ulcers consider taking our wound care certification course and prepare for wound care certification!.

I really appreciate your utilization of the proper terminology regarding the characteristics of venous ulcers. These wounds are unfortunately a common occurrence in our patient population and often presents a challenge due to the chronicity of these wounds.
Laura,
This article was very helpful and informative. I currently have a patient w/ venous ulcers.
Thank you.
Good refresher/overview, appreciated.
thank you Laurie for sending me information i need to understand.
Thanks, Laura~
I am seventy-five years old, and I have been battling a skin disorder that began a few years ago when I helped my relatives move, got all scratched up, and went to sleep in a recliner afterward without cleaning myself up. Bad move.
So, I got cellulitis, for which I got received oral antibiotics and a cleansing regimen and eventually had seventeen days of an antibiotic drip. (PICC line maintenance is a drag, so try to avoid this step, folks.) That cleared it up, but then I started having falls, some of which were pretty traumatic.
Anyway, I have had considerable edema in the ol’ right leg and the resultant venous insufficiency sores. After a lot of trial and error, I seem to be getting pretty good results with an OTC ointment called ActiMaris Wound Gel. I just received an order of 3M Tegaderm Film dressings which come highly recommended. We will see what we will see.
Sorry for the long-windedness, but I am after all a retired English composition teacher. : )
I forgot to add, “Great Website,” which it is. Thank you.
Thanks so much. Good luck with your skin disorder. If you continue to have difficulty, you may want to be seen by a certified wound specialist. To find a specialist in your area visit: https://portal.abwmcertified.org/ABWMweb/Directory/ABWMcontent/Directory.aspx
Hi, I have had many DVTS over the years, mostly in my left leg, and one last year in the Inferior vena cava. I also have May Thurners with varicose veins across the pelvis. About 8mo ago I developed a venous stasis ulcer on my inner ankle. I have another one now only it is above my knee on my left leg. Has anyone else seen this above the knee?
Thanks,
Karen
I recommend that you contact a certified wound specialist to assess your wound. You can search for certified wound specialists in your area here: https://portal.abwmcertified.org/ABWMweb/Directory/ABWMcontent/Directory.aspx
best of luck!