Telemedicine for Wound Care
The pandemic has escalated the need for additional health care options, forcing a new revolution in patient care delivery. With recent world events, the adoption of telemedicine for wound care has quickly risen. Telemedicine is alternatively referred to as teleconsulting, telehealth, virtual visits, or TM.
While we say ‘revolution in patient care delivery’, telemedicine for wound care dates as early as 1990. However, wound care telemedicine has grown at an unprecedented rate in the last few years. Telemedicine has recently given patients access to high-quality wound care while reducing the patient’s risk of viral infections like COVID19.
The refocus of medical professionals during COVID-19 greatly impacted the availability of wound care. Many patients were afraid to enter hospitals and clinics. Wounds were no longer considered a top priority to many. The shortage of staff and space in hospitals also made receiving wound care more difficult.
“The spread of COVID-19 rapidly progressed to become a pandemic event, causing major disruption in health care services, including the care of patients with wounds; Timely wound care is important to prevent complications and reduce the time to healing. Disruption of wound care paradigms [have] led to modifications in the delivery of wound care. ” Dr. Oropallo, MD FACS [2]
The rise in remote technology naturally promoted wound care telemedicine. Today’s smartphones, computers, and video conferencing solutions provide high-quality images and videos that can be utilized for wound diagnosis and management. Currently, twenty-six states have laws requiring private insurers to reimburse healthcare providers for telemedicine services. [1]
Virtual Wound Care through Telemedicine
The visual nature of wounds has made telemedicine an effective choice for wound treatment. Basic wound characteristics like color, location, size, slough, tissue granulation, necrosis, and associated pain can be assessed through telemedicine. A patient’s wound history can be easily conveyed via a virtual visit as well.
Benefits of Telemedicine for Wound Care
There are several additional benefits of wound care telemedicine, notably increased access to high-quality wound care.
Telemedicine makes specialized wound care more accessible to people in rural areas. Rural areas often lack board-certified wound experts, and telemedicine allows patients greater access to these important providers. Even if patients are not living in a rural area, they can benefit from not having to worry about transportation to and from a wound clinic when using telemedicine. This is especially true for elderly patients who may have limited mobility or transportation availability.
Telemedicine providers are also collectively available 24/7, which increases access exponentially. Expanding availability around the clock has greatly reduced the number of emergency room visits, especially from nursing home patients.
Nursing homes, where 24/7 on-site physician coverage is not required, can substitute a telehealth physician for on-call physicians, which allows nursing home patients to receive a quicker consult and potentially avoid hospital admission. [3]
Telehealth is Cost-Effective
Telemedicine is proven to be more cost-effective for both patients and healthcare providers- a mutual win that is often atypical in medicine.
Across all VA patients, telemedicine showed a 25% reduction in bed days and a 19% reduction in hospital admissions. [3]
Telemedicine can also encourage patients to seek out care earlier, which can eliminate more aggressive and costly forms of wound management later.
Telemedicine: A Solution for Chronic Wound Monitoring
Telemedicine has proven to be a viable solution to address frequent wound check-ins. Chronic wounds need more frequent monitoring, and telemedicine can provide the necessary frequency without overburdening patients. Telemedicine may also prevent amputations in patients with chronic wounds, although more extensive research is warranted.
Telemedicine has been used to care for diabetic patients for over two decades with positive results. Most of the studies showed that implementing telemonitoring programs increased the rate of complete ulcer healing. Many additional studies show a comparative outcome for telemedicine patients vs in-clinic patients regarding chronic wounds. [4]
Cons of Telemedicine for Wound Care
Although telemedicine for wound care has many benefits, telemedicine is not an ideal solution for all wounds. There are several limiting factors of telemedicine which include available treatment options.
Telemedicine is not useful in treating severe infections, sepsis, limb-threatening ischemia, or gangrene, to name a few.
Unfortunately, specialized wound procedures like mechanical wound debridement, negative pressure wound therapy, and hyperbaric oxygen therapy cannot be administered through a virtual visit. Additionally, proper wound undermining cannot be adequately measured virtually.
Additional limitations come in the form of physical wound resources available. Many patients may not be able to change their wound dressings alone. Limited wound dressing supplies at home may lead to unsatisfactory alternatives being used, which can complicate wound healing.
Inadequate internet connection or outdated devices (phones, computers, video conferencing systems) can also lead to less reliable imagery or videos, impacting proper telemedicine diagnosis. Elderly patients may additionally have a difficult time adopting new technology without hands-on training.
The Future of Telemedicine
Telemedicine is continuing to evolve, which could eliminate many current barriers discussed above. Advancements in remote monitoring and evolving hospital initiatives will facilitate the growth of telemedicine for wound care.
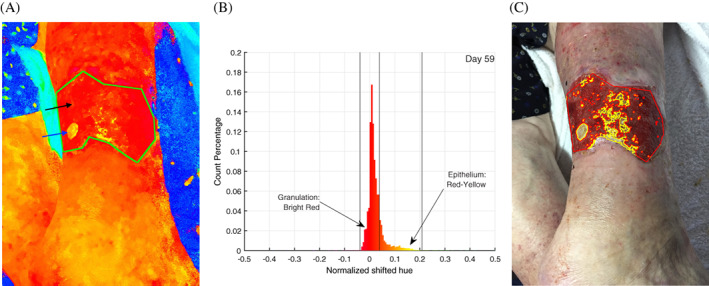
Automated tracking of wound content using images from smartphones is also on the horizon. Wound images taken from a smartphone can be converted to hue‐saturation‐value (HSV) space comprised of three colors – yellow, red, and black. Red shows epithelial tissue. Yellow shows re-epithelialized tissue. The wound imaging algorithm analyzes space and size and can be used to track improvements or declines in wound healing. [5] Continued smartphone technology advances will also lead to more accurate wound depth analysis.
Remote patient monitoring (RPM) will also expand options for telemedicine and home care. RPMs are digital devices or apps that monitor vital signs and health survey responses. The percentage of RPM users is expected to grow 28% by 2024. The Global RPM systems market is projected to be worth over $1.7 billion by 2027, up nearly 128%. [6] Current RPM companies include Dexcom, Honeywell Life Sciences, Medtronic, Philips Healthcare, ResMed, and Senseonics.
Facilities across the country are implementing a “Hospital at Home” or “Hospital Without Beds” program, which focuses more efforts on telemedicine. Early adopter Johns Hopkins in Baltimore, saw a 32% cost reduction compared to traditional hospital visits.
Interested in learning more about telemedicine and wound care?
References
[1] https://www.americantelemed.org/resource/
[2] COVID-19: Issues related to wound care and telehealth management; Alisha Oropallo, MD, FACS
[3]Telehealth: Helping Hospitals Deliver Cost-Effective Care; American Hospital Association.
[4] Telemedicine in Diabetic Foot Care: A Systematic Literature Review of Interventions and Meta-analysis of Controlled Trials.
https://pubmed.ncbi.nlm.nih.gov/29168418/
[5] Towards algorithm-enabled home wound monitoring with smartphone photography: A hue-saturation-value color space thresholding technique for wound content tracking.Shi RB, Qiu J, Maida V.Int Wound J. 2019 Feb;16(1):211-218. doi: 10.1111/iwj.13011. Epub 2018 Oct 31.
[6] Insider Intelligence: Remote Patient Monitoring Industry Explained

How interesting that you talk about the option of telemedicine for wound care. I was just in a small car accident. I will find a good place for wound care nearby.
Tiff,
Hope all is well after your car accident. Sometimes in-person visits aren’t feasible or accessible for all patients. Feel free to fins a wound specialist in your area through this directory. https://abwmcertified.org/find-a-specialist/