Classification of Vasculitis
Vasculitis, an inflammation of the blood vessel wall, is associated with multiple cutaneous manifestations as well as systemic sequelae.(1-5)
Opinions on the Classification of Vasculitis
Opinion is divided over the best way to classify cutaneous vasculitis. Some prefer classification according to etiology, differentiating between primary (idiopathic) and secondary disease.(1) Approximately 50% of cases are idiopathic, while infection (15-20%), inflammatory diseases (15-20%), drugs (10-15%), and malignancy (<5%) are the major secondary causes. However, because multiple causes may contribute to the development of cutaneous vasculitis, a classification scheme based on the size of the diseased vessel is sometimes most useful to the physician.
Small & Medium Sized Vessels
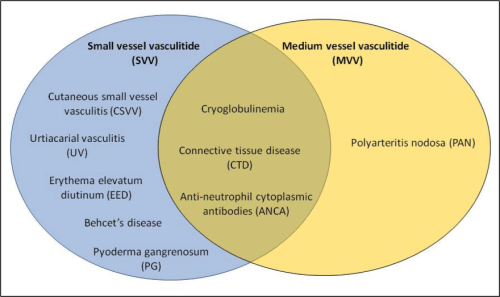
Predominantly small vessel vasculitides (SVV) include cutaneous small vessel vasculitis (CSVV), urtiacarial vasculitis (UV), and Henoch-Schonlein purpura (HSP). Polyarteritis nodosa (PAN) is the only cutaneous vasculitis involving predominantly medium-sized vessels (MVV). Vasculitis associated with cryoglobulinemia, connective tissue disease (CTD), and anti-neutrophil cytoplasmic antibodies (ANCA) involve small and medium-sized vessels. Neutrophilic dermatoses including Behcet’s disease and pyoderma gangrenosum and other skin diseases such as erythema elevatum diutinum (EED) can show evidence of SVV with LCV on biopsy (see Figure).(1)
Cutaneous Findings of Vasculitis
The cutaneous findings of vasculitis depend upon which vessels are primarily involved. SVV most frequently presents as palpable purpura, but can also manifest as urticaria, pustules, vesicles, petechiae, or erythema. Cutaneous signs in MVV include livedo reticularis, subcutaneous nodules, and digital necrosis.(1)
Figure: Classification of primary cutaneous vasculitis based on diseased vessel size (based on Chung and Fiorentino, 2005)1
Classifying cutaneous vasculitis is not straightforward, making diagnosis of the condition somewhat difficult. To learn more about the underlying causes and manifestations of this complex condition, consider studying vasculitis in greater depth as part of a professional wound care qualification.
You can also read our full vasculitis lecture series:
Vasculitis Introduction
Prevention, Diagnosis, and Management of Vasculitis
Vasculitis Summary
Learn More With Our Wound Care Education Options
Interested in learning more about wound care and certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- Chung L and Fiorentino D. Cutaneous Vasculitis. Orphanet encyclopedia, March 2005 (available from http://www.orpha.net/data/patho/GB/uk-cutaneous-vasculitis.pdf)
- de Araujo T and Kirsner RS. Atypical wounds. In: Baranoski S, Ayello EA, eds. Wound Care Essentials: Practice Principles. 2nd Edition. Lippincott Williams & Wilkins, Ambler PA. 2008.
- Panuncialman J and Falanga V. Unusual causes of cutaneous ulceration. Surg Clin North Am 2010; 90: 1161-1180.
- Ferreira MC, Junior PT, Carvalho VF and Kamamoto F. Clinics 2006; 61: 571-578.
- Ball GV, Bridges SL Jr. Vasculitis. 2nd Edition. Oxford University Press, Oxford, UK. 2008.

Thanks for your post and we will certainly try to touch on the topics that you mention in future articles. It is important to note, however that wound care has evolved into such a complex field making it difficult to post a singe article about the topics you mention. (We have an entire 3 hour module that just discusses the various types of wound dressings!) I truly believe that any clinician providing wound care should consider taking a comprehensive course in wound care management and go on to become wound care certified. There are many avenues to achieve wound certification and many employers and clinicians are recognizing the importance of this education.