Vasculitis – Introduction
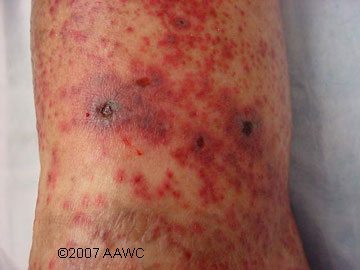
This week sees the start of a new topic as we turn our attention to the condition known as vasculitis. Vasculitis is an inflammation and necrosis of the blood vessels, leading to hemorrhage, ischemia, and infarction. While vasculitis can be triggered by a number of conditions, including diseases of the connective tissue, malignancy, or a drug reaction, the condition can often be idiopathic with no identifiable cause.(1–3)
What is Vasculitis?
Vasculitis is an inflammation of the blood vessels. Vasculitis causes changes in the walls of the blood vessels, including thickening, weakening, narrowing, and scarring. Inflammation can be so severe that the tissues and organs supplied by the affected vessels do not get enough blood. The resulting blood shortage can result in organ and tissue damage or even death.
Many Variations of Vasculitis
The term vasculitis covers a range of conditions which manifest in different ways depending on the size of the blood vessels affected. Systemic effects include fever, joint pain, and malaise. Many of the systemic vasculitis syndromes have a cutaneous component, and patients with small, medium or large-vessel disease may initially present to a dermatologist for diagnosis and management. (4) Vasculitis of the small dermal vessels manifests as palpable purpura, vesiculobullous lesions, and superficial ulcers with regular borders. Vasculitis of the muscular arteries presents as painful red nodules, punched-out irregularly shaped ulcers, or gangrene. (2)
Vasculitis Demographics
Vasculitis affects individuals of all ages, although the young and elderly are disproportionately affected.(4) Because the etiology of the condition is poorly understood, accurate epidemiological studies are difficult to perform, and the true extent of the condition is not well known.(4) However, it seems that there is an ethnic element to the condition, with some races succumbing to certain subtypes of vasculitis more readily than others.(4)
Diagnosis of Vasculitis
As we will see in later weeks, the diagnosis of vasculitis can be problematic and requires a skin biopsy to eliminate other similar conditions. The true diagnosis of vasculitis is made by clinical evaluation and tissue biopsies. Treatment of the vasculitis is based on the extent of the disease. Treatments include the use of systemic steroids, other anti-inflammatory agents or immunosuppressants, among other potential agents. It is important to remember that other conditions such as embolic and Thrombotic diseases can mimic vasculitis. Therefore, a definitive diagnosis should always precede treatment.
Once diagnosed, the underlying causes of the condition should first be addressed, and the lesions managed according to their severity.(5)
More About Vasculitis
If you are interested in studying lesions due to vasculitis, see our full vasculitis lecture series:
Classification of Vasculitis
Prevention, Diagnosis, and Management of Vasculitis
Vasculitis Summary
and other unusual wound presentations in greater depth, you may wish to consider pursuing some form of ongoing professional wound management development. A certification in wound care provides the opportunity to study certain issues in more detail, while also improving your own career prospects.
Learn More With Our Wound Care Education Options
Interested in learning more about wound care and certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- de Araujo T and Kirsner RS. Atypical wounds. In: Baranoski S, Ayello EA, eds. Wound Care Essentials: Practice Principles. 2nd Edition. Lippincott Williams & Wilkins, Ambler PA. 2008.
- Panuncialman J and Falanga V. Unusual causes of cutaneous ulceration. Surg Clin North Am 2010; 90: 1161-1180.
- Ferreira MC, Junior PT, Carvalho VF and Kamamoto F. Clinics 2006; 61: 571-578.
- Ball GV, Bridges SL Jr. Vasculitis. 2nd Edition. Oxford University Press, Oxford, UK. 2008.
- Chung L and Fiorentino D. Cutaneous Vasculitis. Orphanet encyclopedia, March 2005 (available from http://www.orpha.net/data/patho/GB/uk-cutaneous-vasculitis.pdf)

I would love to see something that desribes or defines the unique terminology of wound care. I read these terms used in wound care articles but have found no where to define them. Also an article about when it is appropriate to change the types of dressing and any other items used such as wound gels or the various cleansers as the wound heals. For example I am still using a designated wound cleanser that has antiseptic properties I believe may be preventing the final epithelialization process for a resolving stabe three wound. I think it might be time to switch to normal saline but I am not sure and the specialist treating the patient in the hospital is no longer associated with the patient. The patient’s general physician defers to me for new wound care orders. I really appreciate your responsiveness. Thank you.
I hope in the future CMT and CNA would get an opportunity to certify for wound care or at least take the
course they perform a large part of the ADL’s have a good pulse on longterm care patients. If they could
continue their education and in this way while they are in position of CMT, CNA become a more higher
quality of a caregiver, becoming more knowlegeable in the area of wound care. Would that not slow down
infection issues or at least get treatment started earlier. The professionals can’t do it all many facilities, do
not want to hire or maintain the wages that higher levels of educator or I should say enough and the patient
suffers. If everyone on the unit care team RN, LPN CMT and CNA could recieve similiar education on wound
care. The nurses assistant is envolved on a day to day basis with skin care bathing the patient, keeping skin
clean and applying moisture by the way of lotions, creams, ect. as directed by the care plan of the nuse If they were to recieve such an education perhaps that would relieve some of the stress and strain of nurses in facilities.
It could help with treatment early and consistant care . Usually the RN, LPN ratio on one on one care it greater
per patient and their patient load may be over a whole unit and getting the appropiate consistant wound care
can be challenging and nurses assistant are to help and assist and support them would this not improve the care
that wound care patient recieved if all on the nursing home care unit or home care were educated in this manner
what do you think professional?