Causes and Treatment of Venous Stasis Ulcers
Lower extremity venous stasis ulcers represent approximately 80% of the leg ulcers typically seen in wound care facilities. The following statistics help to bring home the seriousness and chronicity of this common health problem:
- Healing time for venous stasis ulcers averages 24 weeks
- Approximately 15% of these ulcers will never heal
- In 15 to 71% of cases of venous stasis ulcers, the ulcers represent a recurrent lesion
- It is estimated that the cost of treating venous stasis ulcers is 1 to 5 billion dollars every year
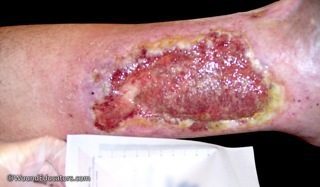
What Causes Venous Stasis Ulcers?
There are two important (and sometimes indistinguishable) causes of venous stasis ulcers. One half to two-thirds of venous stasis ulcers result from progressive disease of the leg veins. The course of such disease is predictable: it starts with the development of varicose veins caused by refluxing of blood within the veins due to incompetent valvular structures. These varicosities may cause variable swelling and discomfort. As disease progresses, skin changes occur (hemosideran staining and dermal and subcutaneous thickening and scarring) which eventually lead to the formation of a venous stasis ulcer. The course of the disease often culminates in ulcer formation in patients in their 60s and 70s.
Approximately one-third to one-half of venous stasis ulcers occur after the patient experiences DVT (deep vein thrombosis). DVTs may cause the process of ulcer formation to occur more quickly than in primary venous insufficiency as described above. Patients who have had a DVT may also present with hemosiderin staining, swelling and discomfort, making it difficult to distinguish post-phlebotic ulcer formation from ulcer formation stemming from venous insufficiency.
How are Venous Stasis Ulcers Treated?
Compression Therapy
Compression therapy is standard in healing venous stasis ulcers; however, before compression therapy is begun, arterial and venous circulation should be evaluated thoroughly to ensure that compression therapy is safe. This can be done by measuring ABIs (ankle brachial pressure index) or by Doppler studies of the lower extremities. Ace wraps are one simple method of compression that can be used, and offers the advantage of ease of application for some patients. Unna boots, which provide compression and wound care together, may also be used. In addition, patients may be measured and fitted for elastic compression stockings. These are commonly used, but may be difficult for some patients to don and doff.
Wound Treatment
The following wound preparations may be recommended:
- Topical or systemic antibiotic therapy for wounds that are infected
- Debridement of exudates and fibrous tissue to stimulate the growth of new epithelium
- Absorbent dressings for heavily draining ulcers
- Acetic acid
- Silver nitrate dressings
- Calcium alginate dressings
- Proteolytic enzyme agents
- Synthetic occlusive dressings
Moist wound healing is the key to healing venous stasis ulcers, facilitating epidermis formation over moist granulation tissue.
Other Treatments
When ulcers fail to heal despite aggressive wound treatment and compression, such as hyperbaric oxygen treatment, skin grafting and systemic therapy with Pentoxyfylline, which promotes blood flow to areas with reduced blood flow (ischemia).
Venous stasis ulcers represent a challenge to healthcare professionals who care for patients with these wounds. A multi-pronged approach is often necessary, including scrupulous wound care, compression therapy and referral to a surgeon when necessary for chronic non-healing wounds.
Learn More With Our Wound Care Education Options
Interested in learning more about wound care and certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- Beylin, M. (2004). Treating venous stasis ulcers in the lower extremity. Podiatry Today, 10 (17). http://www.podiatrytoday.com/article/3038
- Kistner, R., Shafritz, R., Stark, K., & Warriner, R. (2010). Emerging treatment options for venous ulceration in today’s wound care practice. Ostomy Wound Management, 56 (5), pg. 1-11.

Well,actually I took your course. Where are the practice questons?
Hi – what is the current thought on elevating lower extremities with venous stasis ulcers? Is there an appropriate height? higher than heart. I need medical justificcation for elevating leg rests versus tilt in space in a power chair. Always a challenge.
Hi Joan, elevation higher than the heart is ideal, however it is important to discuss your situation with your doctor. If you have any heart issues or similar medical conditions elevation is not always recommended.
I would like to learn more about draining ulcers and what to approach my
m d with . I am a retired r n and I have stasis ulcers and i am using.the unna boot at present. I also have chf
I recommend contacting a certified wound specialist for an evaluation.