Types of Wound Debridement
Debridement is the removal of foreign material, devitalized tissue, or contaminated tissue from the wound bed. Debridement is an important procedure that greatly affects how a wound will heal. Necrotizing tissue has a negative effect on wound healing. Removal by medical intervention is often necessary. Many wound dressings provide sufficient debridement without further intervention.
Wound healing is a highly integrated cellular event. As a result, many factors must be analyzed before deciding if debridement is a viable option for your patient. There are several methods of debridement including surgical, enzymatic, autolytic, mechanical, and biological.
When selecting any dressing or debridement technique, make sure to analyze:
- The location of the wound
- The wound bed
- The wound depth
- The periwound skin
- Vascular health
- The wound occurrence (is it chronic?)
- Who will be changing the wound dressing
- Patient nutrition
The drainage and depth of the wound should dictate the type of dressing and debridement method chosen. It should also suit the condition of the periwound skin. Wounds that are poorly vascularized should not be debrided. The location of the wound will determine the suitable thickness of the dressing and the extra protection it may need. Patient adherence, including nutrition, self-administered dressing changes, or healing disruptions should also be considered.
Types of Debridement
The types of debridement are broken out into two categories based on how they affect tissue. Selective debridement targets the devitalized tissue only while non-selective targetsthe entire wound, including healthy tissue.
- Surgical Debridement (Sharp = Selective)
- Enzymatic Debridement (Selective)
- Autolytic (Selective)
- Biological (Selective)
- Mechanical (Nonselective)
- Irrigation (Nonselective)
Surgical Debridement
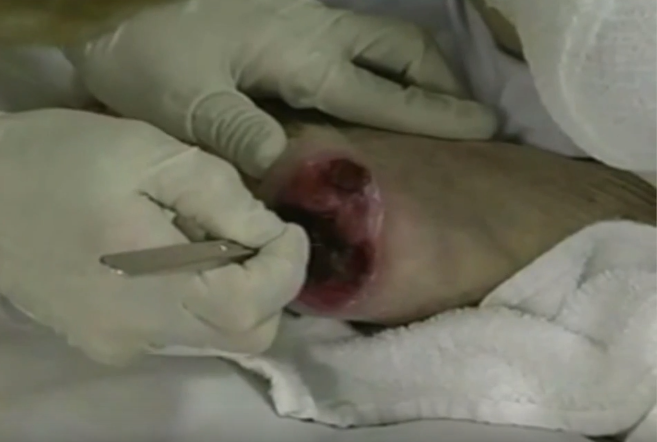
Enzymatic Debridement
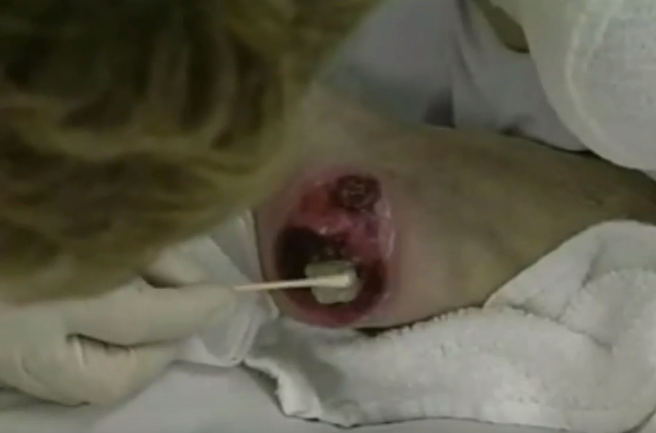
Enzymatic debridement utilizes chemical agents to break down necrotic tissue. Typically, the enzyme is combined with a dressing that is changed regularly, which softens the tissue and allows for the necrotic tissue to be removed when the dressing is removed.
Some of the advantages to enzymatic debridement are:
- Works faster than autolytic debridement
- little risk to healthy tissue when properly applied
Some of the disadvantages to enzymatic debridement are:
- The patient must have the chemical agent prescribed and it may be relatively expensive
- It is important to ensure healthy tissue does not come in contact with the chemical agent
- A secondary dressing may be required to absorb exudate
- Enzymatic debridement may cause some discomfort to the patient (i.e., burning sensation, increased wound pain)
Many practitioners employ enzymatic debridement after surgical debridement for chronic wounds.
Autolytic Debridement
Autolytic debridement uses the body’s own defense mechanisms and fluids to liquefy eschar, slough, and other forms of necrotic tissue. Autolytic dressings are non-adherent and help promote healthy tissue growth and natural enzyme formation. Hydrogels, hydrocolloid dressings, alginates, hydrofibers, and transparent films are autolytic debridement dressings. These dressings are virtually pain-free because they do not disrupt or stick to the wound bed.
In addition to patient tolerance, another benefit of autolytic debridement is the relatively low cost compared to more extreme debridement techniques. Autolytic debridement is very common in long-term wound care because they encourage the body to try to heal itself.
Choosing the RIGHT Autolytic Dressings
Hydrogels and hydrocolloids may cause maceration of the periwound skin, making them a poor choice for high-drainage wounds. Alginate dressings are another form of autolytic debridement dressings. Alginate dressings can prevent maceration, which makes them a better choice for high-drainage wounds. Autolytic debridement is also not recommended for infected wounds.
Misdiagnosis when Using Autolytic Wound Dressings
With autolytic dressings, it is important not to mistake liquified necrotic tissue for purulent drainage, as the color and odor may be characteristically similar.
Mechanical Debridement
Wet-to-dry dressings, such as wet gauze dressings, are the most common mechanical debridement treatment. Wet gauze treatments are also a treatment option for some necrotizing wounds because they pull necrotic debris out of the wound and transfer it into the gauze.
The downsides to mechanical debridement include potential disruption of newly formed tissue. Wet-to-dry debridement may reopen healing wounds. Removal can also be painful for some patients. Compared to other debridement techniques, this one is relatively slow. Many providers often combine mechanical debridement and autolytic debridement to speed up healing and reduce further tissue damage.
Biological Debridement
Biological debridement is the use of other organisms to facilitate debridement. The most well-known example is maggot debridement. One benefit is precision- maggots are able to consume necrotic tissue more accurately than a human eye can judge removal. One of the downsides to biological debridement is patient pain. Another downside is organism availability since this is not a common practice.
Irrigation Debridement
Irrigation uses fluid to remove wound debris topical agents, and surface bacteria. While some do not consider irrigation to be one of the core debridement categories, it is still a common debridement method. This is often followed by another method of debridement. Irrigation is a non-selective debridement technique that is quick and cost-effective.
Choosing the Best Debridement Technique
Wound debridement is not a one-size-fits-all remedy. Many chronic wounds require combined wound therapy.
Consider all aspects of the wound, including the wound bed, depth, periwound skin, present drainage, and vascular health. Also consider patient nutrition, and who will be responsible for changing any wound dressings. Patient adherence and healthcare provider’s debridement knowledge can greatly impact the prompt healing – or further decay and recurrence – of a wound.
More Resources About Debridement:
Methods of Debridement:
Wound Bed Preparation
Serial Debridement Evidence
Debridement Training
Debridement Techniques:Biological Debridement
Debridement Techniques: Surgical Debridement
Debridement Techniques: Sharp Debridement
Debridement Techniques: Mechanical Debridement
Debridement Techniques: Enzymatic Debridement
Debridement Techniques: Autolytic Debridement
Sources:

Would th ou s training certify me to be able to do mechanical debriedment?. I am an en with an associates degree.
Thank you
Jacinta
Jacinta,
You can use any of the following free resources on our site to learn more about debridement. All of our online wound care certification courses – available for purchase here – https://woundeducators.com/wound-care-certification-courses/ – will teach you all the debridement basics and techniques. In order to become wound care certified, you must review the full eligibility of the wound care certification you wish to pursue- the ABWM offers the CWS, CWSP, and CWCA certifications; the WOCN and CWCN are offered by the WOCNCB, and the WCC is offered by NAWCO.
What recommendations/ support do you give or provide to an individual (RN ) in order to obtain the 1500 hours of hands on training/monitoring which is required to sit for the CWCN exams ? I’m speaking specifically of a preceptor.
Hi Lorrestine, we recommend searching for preceptors here: https://www.wocn.org/page/Nurse_Referral
If you have more questions, email us at [email protected].