Phototherapy in Wound Management
Phototherapy, also known as light therapy, has been used in a healing and medical context since prehistoric times. These days, the source of light energy tends to be dedicated, custom-made medical equipment rather than the sun, but the general principle remains much the same.
Ultraviolet (UV) light phototherapy has also been used to treat a variety of skin conditions including open wounds, while evidence suggests that the modality may also have a role in preventing or controlling infection in orthopedic surgical wounds.1-3 UV radiation is known to promote exfoliation of the outer skin layers, enhance healing through the induction of an erythematous response in the skin, and inactivate a variety of microorganisms. Short-wavelength UV light is also being investigated for the treatment of infected acute and chronic wounds along with its putative ability to stimulate wound healing.1,4
As well as UV light, evidence suggests a benefit of other sources or light energy, such as light emitting diodes, laser diodes, superluminescent diodes, or a combination of these sources, in wound healing.5-8 Biologic effects of these light sources include increased cellular proliferation and differentiation, increased mitochondrial production of ATP, increased RNA synthesis, and increased the release of chemotactic factors from mast cells.
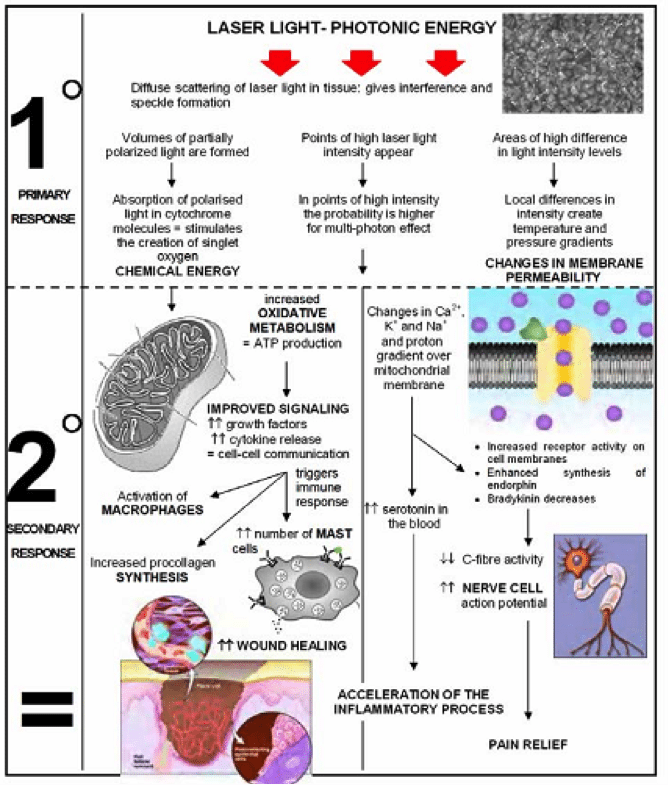
Although the exact mode of action of phototherapy is not fully understood, it is believed principally to involve an interaction between photons and molecules in the tissues as well as secondary mechanisms that relate to the effect of the chemical changes induced by this primary effect (see Figure).7
To date, few controlled, randomized studies into the potential benefits of phototherapy have been conducted to date. Furthermore, there is still little standardization in the application of phototherapy, which makes a full assessment of this modality problematic.7 However, there is a wealth of anecdotal evidence for the effectiveness of phototherapy in wound management, while preclinical studies have been able to suggest a plausible mechanism for a benefit of action.7 Nevertheless, until definitive data are available in this area, phototherapy is likely to remain on the fringes of mainstream wound management.
References
- Sussman C and Bates-Jensen B. Wound Care: A Collaborative Practice Manual for Health Professionals. 3rd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007.
- Brown S. Clinical Antimicrobial Photodynamic Therapy: Phase II Studies in Chronic Wounds. J Natl Compr Canc Netw 2012;10 Suppl 2: S80-3.
- Thakuri PS, Joshi R, Basnet S, Pandey S, Taujale SD, Mishra N. Antibacterial photodynamic therapy on Staphylococcus aureus and Pseudomonas aeruginosa in-vitro. Nepal Med Coll J 2011 13: 281-4.
- Onigbinde AT, Adedoyin RA, Ojoawo OA. Effects of ultraviolet radiation (type B) on wound exudates, appearance and depth description. Technol Health Care 2010; 18: 297-302.
- Dawood MS, Salman SD. Low level diode laser accelerates wound healing. Lasers Med Sci 2012 Aug 16. [Epub ahead of print]
- Paschoal MA, Santos-Pinto L. Therapeutic effects of low-level laser therapy after premolar extraction in adolescents: a randomized double-blind clinical trial. Photomed Laser Surg 2012; 30: 559-64.
- Hawkins D and Abrahamse H. Phototherapy – a treatment modality for wound healing and pain relief. African J Biomed Res 2007; 10: 99-109.
- Chandrasekaran B, Chettri R, Agrawal N. Short-term multimodal phototherapy approach in a diabetic ulcer patient. Singapore Med J 2012;53: e122-4.
Learn More With Our Wound Care Education Options
Interested in learning more about wound care and certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.