Preventing Heel Pressure Ulcers
Heels are particularly vulnerable to skin breakdown due to the fact that the posterior heel is covered only by a thin layer of skin and fat. When patients lie supine, all of the pressure of their lower legs and feet rest on the heels, which have relatively poor skin perfusion and a paucity of muscle tissue to absorb stress.
Prevalence rates for heel pressure ulcers vary, but have been estimated to be as high as 25% across a mixture of continuing care and acute care settings. Heel ulcers represent approximately 1/3 of pressure ulcers acquired, resulting in increased morbidity and mortality. In some cases, heel pressure ulcers can lead to amputation of the affected limb.
What Are the Risk Factors Associated With Heel Pressure Ulcers?
Several known factors increase a patient’s risk of developing a heel pressure ulcer, including:
- Inadequate/malnutrition
- Advancing age
- Abnormalities of circulation
- Sensory deficiency
- Immobility
- Major surgery
- Multiple health problems (comorbidities)
- Dehydration
- Friction and shear forces
- Diabetes
- Peripheral vascular disease
- Hip fractures
- Low albumin levels/anemia
- Obesity or low body-mass index
The above factors can be applied to all pressure ulcers, not just those affecting the heel.
Clinical Presentation of Heel Pressure Ulcers
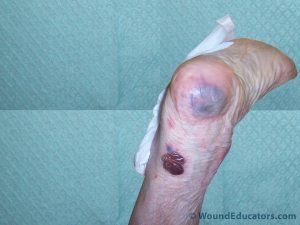
In the beginning, heel pressure ulcers may present with tenderness, discoloration of the skin and changes in skin temperature over the affected area. Heels that present with non-blachable erythema evidence decreased perfusion to the area, which may be due to friction or shearing forces or injury related to pressure. Deep tissue injuries may be recognized as areas on the heel that are dark purple or reddish-purple in color, boggy or firm and warmer or cooler to touch than surrounding tissue. The area will likely be tender and may develop blisters filled with blood or serum. As conditions deteriorate, the blisters may dry and become black in color (eschar); an open wound may develop from the area. (Remember that deep tissue ulcers are a special category of pressure ulcers and cannot be staged).
Preventing Heel Ulcers
The best offense is s good defense, and this saying holds true for preventing heel pressure ulcers. Preventing heel ulcers begins with anticipating that they may occur when patients have one or more of the listed risk factors and are supine for any length of time. How are pressure ulcers prevented? The following can be used to prevent heel pressure ulcers from developing:
- Pillows- pillows can be used for offloading heel pressure in cooperative patients for short periods of time, according to the NPUAP. It is recommended that pillows be placed length-wise under the calf to completely elevate the heel off the supporting surface. It can be difficult to maintain proper positioning when patients move around in bed, which is the reason that the NPUAP recommends this treatment modality only for cooperative patients, and only for short duration.
- Heel offloading devices- devices made of sheepskin, splints and bunny boots are all acceptable offloading devices which can stay in place around the clock and can be used for all patients, regardless of how much they move in bed. These devices pad the heel and prevent friction and shear; they also remove some pressure from the heel, preventing heel pressure ulcers.
Heel pressure ulcers can cause significant morbidity and mortality. They should be anticipated and prevented in patients at risk for pressure ulcers. Preventing heel ulcers involves the use of simple devices such as pillows and offloading devices to protect delicate heels.
Learn More With Our Wound Care Education Options
Interested in learning more about wound care and certification? Browse through our wound care certification courses for information on our comprehensive range of education options to suit healthcare professionals across the full spectrum of qualifications and experience.
References
- Fowler, E., Scott-Williams, S. & McGuire, J. (2008). Practice recommendations for preventing heel pressure ulcers. Ostomy Wound Management, 54(10).
- Langemo, D., Thompson, P., Hunter, S., Hanson, D. & Anderson, J. (2008). Heel pressure ulcers: Stand guard. Advances in Skin and Wound Care, 21(6), pg. 282-292.
