Wound Bed Preparation- Exudate Management
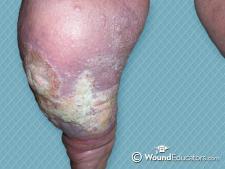
Moisture balance in the wound bed is essential to wound healing. The body produces exudate as a response to tissue injury, and the amount of exudate is dependent upon the pressure gradient within the tissue itself. Wounds must be moist enough to promote cell growth and proliferation, as well as support the removal of dead tissue through the process of autolysis (a form of chemical debridement using the body’s own fluids). Wounds in which exudate is excessive may become macerated, which can lead to further tissue damage and set the stage for infection. This can occur in wounds that are infected, or in wounds that are stalled in the inflammatory phase of healing.
Exudate in Acute and Chronic Wounds
Exudate (wound fluid) typically differs in acute versus chronic wounds. In acute wounds, exudate is rich in nutrients and leukocytes, which stimulate fibroblasts and endothelial cells to replicate. In chronic wounds, however, high levels of proteases, which slow cellular proliferation, are found. In addition there is often poor growth factor activity, which leads to a lack of development of the wound matrix, which in turn means that epithelial cells cannot migrate across the wound surface to complete the wound healing process.
Factor Affecting Wound Exudate Production
Many factors can influence the production of wound exudate, including:
- general patient condition
- type/etiology of wound
- dressing selection
- Presence of infection
- desiccation of the wound bed
- maceration
Assessment of Exudate
Wound exudate can be described according to the following four characteristics/descriptors:
- Type- Exudate can be described as serous, sanguinous, both serous and sanguinous (serosanguinous), purulent or seropurulent. Serous or sanguinous drainage (or a combination of the two) is normal, while seropurulent or purulent drainage is often a sign of infection.
- Color- Normal wound drainage is clear or pale yellow in color; red or dark brown drainage signifies old or new bleeding. Wounds that have a distinctive blue-green drainage present often have Pseudomonas
- Consistency- wound drainage consistency may be thin and watery or thick. Thick drainage hints at the possibility of infection.
- Amount- Most wounds will have some drainage present. Wounds that have no exudate at all are often desiccated or necrotic. Minimal to moderate exudate should be considered normal, providing the amount of drainage is not disproportionate to the amount of necrotic tissue present, which could signify that infection is present. A copious amount of exudate should raise a concern about the presence of infection.
Selection of Dressing for Exudate Management
Wounds that are too dry require a dressing that will donate moisture, while wounds that are too moist will require a dressing that will absorb exudate and wick it away from the skin to prevent breakdown. There are many dressing available on the market; dressing selection should be based on the amount and viscosity of wound exudate. Dressings to manage wound exudate may include hydrocolloids, foams, hydrofibers, alginates, capillary action dressings and cadexomer iodine.
Other Treatments to Manage Exudate
For wounds with heavy exudate, vacuum dressings which use an electronic pump to pull fluid from the wound bed can be used. For patients with venous stasis ulcers, compression bandages can be used to decrease fluid in the lower extremities. Skin barrier creams and films can help protect the periwound area from becoming excoriated or macerated due to excess exudate.
If you enjoy reading and learning about the principles of wound bed preparation and exudate management, perhaps it’s time to think about pursuing a career as a certified wound care professional. Wound Educators is the premier wound care education website for online wound care learning.
Editors Note: This post was originally published in December 2007 and has been revamped and updated for accuracy and comprehensiveness.
Source:
Dowsett, C. & Newton, H. (n.d.). Wound Bed Preparation: TIME in Practice. Wounds International.
Dowsett, C & Schultz, G. (2012). Wound bed preparation revisited. Wounds International, February 3(1).

I really enjoy reading ur articles, they are very educational…thank you for sharing you’re knowledge..
I enjoy the knowledge of this organization and I hope to carry the awesome title of wound care certification this stage of my Nursing career
Hi Marcia,
Thank you for your interest in WoundEducators.com.
If you are leaning toward a course that will eliminate the need for travel and work absences, then the WoundEducators.com online course is perfect for you. It will also allow you to proceed at your own pace with a high level of learning and retention.
I was researching about this Wound Exudate Production. Thanks a lot for the valuable knowledge. It’s really helpful.
I find this interesting and am eager to learn more as I go through the wound course I am taking.
Thank you for the feedback, Teri! If you have any other topics you would like to see on our site in future blogs, let us know!
Outstanding post, I conceive website owners shoujld larn a lot from this blog its rattling user friendly.
So muhh good information on here :D.
I ddo not even understand how I finished up right here, however I assumed this
publish was once great. I do not recognise who you are however certainly you are
going too a well-known blogger should you are not already.
Cheers!