MRSA Infected Wounds: A Study Involving Oakin® Antimicrobial Dressings

Wound care practitioners are no doubt aware that the incidence of MRSA infected wounds in the community is increasing, resulting in new challenges in wound management. A study that appeared in the Journal of Wound Care (February, 2014) describes a new approach to the treatment of wounds infected with MRSA using a dressing derived from natural tannins and incorporating components of the de-escalation theory.
De-escalation Theory of Antimicrobials
The de-escalation theory can be defined as “the streamlining of empirical antimicrobial therapy based on the culture results for severe infection…which can more effectively target the particular causative pathogens which results in decreased antimicrobial exposure” (Graham & Bhatia, 2014). The theory considers the patient’s risk factors for MRSA, including:
- recent/current hospitalization
- geographic location
- living in a long term care facility
- prior history of infection/colonization with MRSA
- presence of invasive devices
- association with health care workers
- chronic illness
- living in crowded/unsanitary housing/conditions
- treatment with antibiotics within the past year
- immune system disorder or weakness
- age (younger or older in age)
- participating in sports/sharing towels or athletic equipment
In addition to determining the patient’s individual risk factors for MRSA, de-escalation in terms of the study discussed here considers the following important points:
- cultures should always be obtained of any sites suspicious for infection prior to antibiotic therapy
- the initial empiric therapy chosen should be based on most likely pathogen suspected, cost-effectiveness and impact on the potential development of antibiotic resistance
- any recent antibiotic therapy should be considered, as it may have altered the patient’s normal flora
- patients who are immune compromised or who are severely ill may require broader empiric antibiotic coverage
In essence, this theory serves to encourage practitioners to carefully consider whether antibiotics are necessary and, if they are deemed necessary, which antibiotic(s) should be chosen based on the factors listed above.
Oakin Wound Dressing Info
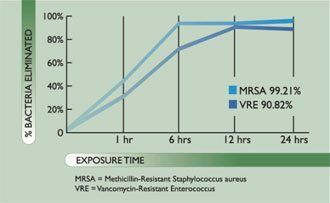
Today’s wound dressings may contain a variety of antimicrobial agents, including ionized silver, iodine, polyhexamethylene biguanide (PMB) and tannins. Oakin is a natural tannin made from oak extract. It is known to be effective against 51 bacterial and fungal pathogens, including VRE and MRSA. The AmeriGel Wound Dressing, manufactured by Amerx Health Care Corporation, is designed to be used on wounds that are hydrogel-appropriate: in other words, wounds that do not have exudate, wounds that are dry and require moisture, or wounds that have only minimal exudate.
Lower Extremity Wound Study
Study authors G.S. Graham & A. Bhatia developed a protocol to treat lower extremity wounds infected with MRSA and caused by various etiologies: pressure ulcers (7 participants; 17%), venous insufficiency ulcers (10 participants; 25%), and diabetic neuropathic ulcers (23 participants; 58%). The study participants (n=40) had a single lower extremity wound that was culture positive for MRSA and was hydrogel-appropriate.
After giving informed consent, wound cultures were obtained from participants who presented with classic signs of infection (erythema, edema, warmth, pain and purulent discharge or exudate). All participants who took part in the study were evaluated for their risk factors for MRSA, according to the risk factors listed above. Participants were evaluated and treated according to a protocol designed by the author, which included:
- sharp wound debridement (performed every 7 to 14 days, depending on the wound care setting)
- wound culture
- antibiotic therapy (when appropriate)
- daily dressing change using Oakin antimicrobial hydrogel (performed by patients or their caregivers after necessary teaching and provision of a wound care instruction sheet)
Antibiotic therapy was reassessed once wound cultures were available to ensure that the identified pathogens were covered appropriately. Oral antibiotics were added according to the patients’ allergies, comorbidities, vascular condition, insurance coverage/ability to pay and drug resistance if wounds failed to improve. Participants were followed for 12 weeks and wounds were reassessed at 30, 60 and 90 days, or until wound closure was achieved.
The results of the study revealed the following:
- 35% of the wounds healed in 30 days, 60% in 60 days and 78% in 90 days (after 90 days, the remaining participants were no longer followed)
- 10% received no empiric therapy (their only treatment was the Oakin antimicrobial wound dressing)
- the Oakin dressings were well tolerated, and none of the participants experienced an allergic or adverse reaction
This was a small study; obviously, larger studies are needed to verify results. However, the results indicate that this protocol utilizing Oakin antimicrobial dressings was effective for treating individuals with lower extremity wounds infected with MRSA.
“Oakin® promotes faster healing in wounds such as diabetic skin ulcers, pressure ulcers, venous stasis ulcers, scrapes, cuts, rashes and resolves skin irritations caused by bacteria and fungus. The unique benefits of Oakin® have earned Amerigel® Wound Dressing high ratings for topical wound / ulcer treatment by wound care professionals.”
Source:

Thank you for the email.
You are welcome Lucy. I hope that you found the article useful.
hello, I just read the article about MRSA and studies involving wound healing. the article marketed Amerigel as as the number one dressing of choice. I am wondering if this is marketing based on selling this product or if this is the recommendation by the wound care institute?
thank you…Laura Jones RNC,WCC
Hi Laura, Thank you for posting. We are not affiliated with the Wound Care Education Institute so I cannot speak for them. At WoundEducators.com we strive to present unbiased factual information based on evidence based medicine. At this time Amerx is the sole manufacturer of the Oakin® based products and has been discussed for that reason.
Hi Laura. Thanks for this wonderful useful information regarding this new wound dressing specifically for infection wounds. I wonder if this is already available here in Saudi Arabia. Also, I am hoping that soon you will also post on topics regarding leg ulcers, cellulitis, its intervention and treatment. Just one question: who should be the first to see case of cellulitis-general surgeon, vascular surgeon or plastic surgeon?
Thank you.. Myla Clarissa C. Rivera, BSN, RN, WCN
Hi Myla, I recommend that you contact Amerigel to see if there product is available in Saudi Arabia. In the case of cellulitis it is essential that the infection is resolved first!
Hi Lauries;
Thanks for such wonderful topic for wound-care givers we really appreciate, MRSA is such a challenge in all fields and not easy to deal with, my question is do you think debridement had a major role in the treatment and then is amerigel ( oakin) a chemical debrider or how do you classify it . Is the Oakin available in Kenya or how can i get the supply.
Hi Ezekiel, Thank you for your comment. Yes, debridement of devitalized tissue plays a major role in wound healing. Oakin is considered a form of enzymatic debridement. For more information about Oakin visit AMERIGEL.