Wound Assessment: Assessing the Periwound and Surrounding Skin
In addition to noting the characteristics of the wound itself, clinicians should also examine the periwound and the surrounding skin, comparing this tissue to the skin outside the affected area, as well as comparing the opposite (contralateral) side where possible.
Structure and Quality
When assessing the periwound and surrounding skin, the following should be noted:
- Condition of the skin- Note whether the skin appears to be thin, transparent or fragile, and thus prone to tearing
- Hydration- Note whether the periwound tissue is dry, flakey or cracked, signalling that there is too little moisture present, or whether the periwound tissue is overly moist or macerated. Tissue turgor can be assessed by gently grasping the surrounding tissue between the thumb and forefinger and allowing it to return to its natural position. If there is a delay, this may signal dehydration of the tissue; however, it is natural for aging skin to be slightly delayed in returning to its normal contours.
- Skin abnormalities-Note the presence of any scars, deformities, rashes, varicosities or other skin abnormalities that may hint at previous skin conditions or underlying health conditions that may affect wound healing.
Color
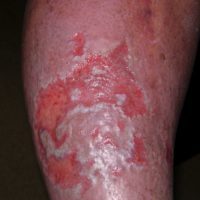
The color of the periwound and surrounding skin can yield clues that can help you assess potential problems. A certain amount of erythema (redness) is expected and indicates inflammation; however, when there is more erythema than you would expect, infection should be suspected. Note whether the erythematous tissue is nonblanchable should lead you to suspect that ischemic damage may be present, possibly due to pressure that has been sustained and unrelieved. Skin that is lighter in color than the surrounding skin may represent tissue that does not have a robust supply of blood, or it might indicate scar tissue that is new and has not yet regained normal skin coloration. Skin that is dusky in color may represent an area of severe ischemia. Hyperpigmented skin may be caused by venous insufficiency of longstanding duration.
Hair and Nail Growth
Denuded areas of skin may indicate that the area in question lacks adequate blood supply i.e. ischemia. This is often readily apparent in the lower legs. Fungal infections affecting the toenails often coincide with ischemic changes. Of course, the presence or absence of ischemia should be verified with testing, but hair and nail abnormalities will often be found when ischemia is a problem.
Edema
The presence of pitting edema should be quantified using an accepted scale, typically a scale from 1 to 3+ or 1 to 4+, indicating minimal to severe edema. Edema that has been present for a long time will often be nonpitting and this indicated that the tissue is fibrosed. Limbs should be measured circumferentially, which allows for ease of reassessment. The limb can be marked so that the clinician knows where to place the measuring tape at the next assessment, or specific landmarks can be used and referenced so that measurements are taken at the same place each time. For example, the tibial tuberosity can be used as a landmark and measurement can be taken at a prescribed distance distal to this landmark.
Temperature
The back of the hand can be used as a gauge to determine whether skin temperature is the same, increased or decreased in relation to nearby, unaffected areas, as well as the contralateral side. An increase in temperature may indicate an infection is present, while a decrease in temperature may indicate a lack of blood flow to the area. Because temperature is so subjective, it should be used in conjunction with other assessment findings
As can be seen, assessment of the periwound and surrounding skin is an important part of wound assessment and should never be neglected, as the information that can be gleaned from examination of these areas can provide a wealth of information regarding the potential and status of wound healing, as well as the presence or absence of infection or other conditions.
If you would like to learn more about wound assessment and wound care management, visit Wound Educators to learn how you can become a certified wound care specialist.
Source:
Meyers, B (2008). Wound Management: Principles and Practice. 2nd edition. Pearson Prentice Hall. Upper Saddle River, New Jersey. pg. 56-57.
Bryant, R & Nix, D. Acute and Chronic Wounds: Current Management Concepts. 4th edition. Elsevier Mosby, Saint Louis, Missouri. pg. 117.

Ok ,I have shin around my Larvix after surgery years ago,22 years ,I also have COPD ,how to get Drs, to study and do more infections etc?
I recommend that you contact a certified wound specialist to assess your wound. You can search for certified wound specialists in your area here: https://portal.abwmcertified.org/ABWMweb/Directory/ABWMcontent/Directory.aspx
best of luck!
Can please send me wound tips weekly. Thanks.
Allison, have you signed up for our newsletter yet? That is the best way to get updates!
My name is Susana obeng I’m certified wounds care certified and I will like to apply to any of your facilities why I can get y hands ✋on I need be treatment , K
Susana,
You can find wound care jobs that may fit what you are looking for on our job board – Wound Care Jobs
best of luck, and thank you for your commitment to wound care!